Tue, May 19, 2026
Volume 10 - Continuous Publishing
Iran J Neurosurg 2024, 10 - Continuous Publishing: 105-115 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Khoshsima N, Jafari S, Alijani B, Behzadnia H, Homaei Rad E, Yousefzadeh- Chabok S et al . The Association of the Changes in Pain Severity and
Cervical Cobb Angle before Versus After Anterior Cervical
Discectomy With Fusion Surgery. Iran J Neurosurg 2024; 10 : 12
URL: http://irjns.org/article-1-423-en.html
URL: http://irjns.org/article-1-423-en.html
Naghmeh Khoshsima1 

 , Seifollah Jafari *2
, Seifollah Jafari *2 

 , Babak Alijani3
, Babak Alijani3 

 , Hamid Behzadnia3
, Hamid Behzadnia3 

 , Enayatollah Homaei Rad4
, Enayatollah Homaei Rad4 

 , Shahrokh Yousefzadeh- Chabok5
, Shahrokh Yousefzadeh- Chabok5 

 , Zoheir Reihanian3
, Zoheir Reihanian3 




 , Seifollah Jafari *2
, Seifollah Jafari *2 

 , Babak Alijani3
, Babak Alijani3 

 , Hamid Behzadnia3
, Hamid Behzadnia3 

 , Enayatollah Homaei Rad4
, Enayatollah Homaei Rad4 

 , Shahrokh Yousefzadeh- Chabok5
, Shahrokh Yousefzadeh- Chabok5 

 , Zoheir Reihanian3
, Zoheir Reihanian3 


1- Guilan Road Trauma Research Center, Trauma Institute, Guilan University of Medical Sciences, Rasht, Iran. & Department of Neurosurgery, School of Medicine, Poursina Hospital, Guilan University of Medical Sciences, Rasht, Iran.
2- Department of Neurosurgery, School of Medicine, Poursina Hospital, Guilan University of Medical Sciences, Rasht, Iran. ,jafariseifolla@gmail.com
3- Department of Neurosurgery, School of Medicine, Poursina Hospital, Guilan University of Medical Sciences, Rasht, Iran.
4- Social Determinants of Health Research Center, Trauma Institute, Guilan University of Medical Sciences, Rasht, Iran.
5- Neuroscience Research Center, Trauma Institute, Guilan University of Medical Sciences, Rasht, Iran.
2- Department of Neurosurgery, School of Medicine, Poursina Hospital, Guilan University of Medical Sciences, Rasht, Iran. ,
3- Department of Neurosurgery, School of Medicine, Poursina Hospital, Guilan University of Medical Sciences, Rasht, Iran.
4- Social Determinants of Health Research Center, Trauma Institute, Guilan University of Medical Sciences, Rasht, Iran.
5- Neuroscience Research Center, Trauma Institute, Guilan University of Medical Sciences, Rasht, Iran.
Full Text [PDF 1599 kb]
(708 Downloads)
| Abstract (HTML) (2834 Views)
4. Discussion
Considering that degenerative neck diseases have a high prevalence and ACDF surgery is one of the common surgeries in neurosurgery patients, and also considering that sometimes patients still mention axial neck pain after surgery, it is felt necessary to conduct some studies for finding possible causes of this pain and to provide solutions to remove it. Therefore, in this research, an attempt was made to take a step in this direction by examining the Cobb angle before and after surgery and its correlation with axial neck pain following operation.
One limitation encountered in this study was the usual practice of obtaining pre- and post-surgery lateral cervical X-rays with patients lying down, given pain relief and immobility with a hard collar after surgery. To address this issue, requests were made to the radiology unit for standing X-rays in weight-bearing conditions to enhance the accuracy of C2-C7 Cobb angle calculation.
Another challenge was that some patients had no access to communication tools and medical facilities for the third and fourth visits, after entering the study and providing their information at the pre-surgery and immediate post-surgery visits, leading to their exclusion from subsequent comparisons within the study population.
Furthermore, some patients had printed neck X-rays or no access to the hospital’s PACS system, making it difficult to import the image into the Surgimap software for Cobb angle calculation.
The first result of this research shows that the average pain score after the operation has decreased significantly compared to before the operation and this difference was statistically significant. This difference was evident until the second and sixth months after the operation. This result is also confirmed in other research in this field that ACDF is associated with a clear reduction of axial neck pain in patients who have undergone surgery, especially for the treatment of myelopathy or radiculopathy. In a recent meta-analysis by Harrop et al. [12], patients with neck pain predominant had a greater reduction in neck pain after surgical fusion with a change from a baseline of 53.4%. In another study by Riew et al. [13], a mean improvement of the pain of at least 50% was observed approximately 4 years following surgery. In their study, functional outcomes improved between 32% and 52% from baseline. In another systematic review and meta-analysis by Oitment et al. [14], the individual neck pain mean differences were reduced at different time points after surgery from 6 weeks to 48 months of follow-up. Therefore, it can be said that for the management of patients’ axial neck pain due to DCM, ACDF surgery can be an option of choice for these patients.
As another critical result, the mean absolute value of the Cobb angle increased after surgery compared to before surgery, and this difference was statistically significant. This increase was evident until the second and sixth months after the operation. Also, the results of this study show that the average changes in the Cobb angle of each measurement period after the operation (two to six months after the operation) were statistically different from before the operation and this trend was decreasing. However, we found no relationship between neck pain with Cobb angle in different time points, which could potentially be influenced by our small sample size. However, in the investigation of the possible influence of other background indicators, such as age, sex, cage size and duration of disease symptoms, the relationship between pain and angle changes remained non-significant. In an article published by Yuan Cao et al, 144 zero-profile ACDF patients were examined, of which 48 had axial neck pain after surgery. The patients were followed up for one year and they finally concluded that the C2-C7 Cobb angle before surgery is a risk factor for severe axial pain after surgery in zero-profile ACDF patients [15]. Similarly, in a retrospective cohort study by Canseco et al. 308 patients who underwent ACDF at one to three levels were examined, and found that patients in whom the C2-C7 Cobb angle was corrected to a neutral or lordotic position had more axial neck improvement as compared to patients with the kyphotic state [16]. In Liu et al. study on 88 patients who were followed for one year, it was found that preoperative neck pain severity and kyphosis status can predict the severity of postoperative neck pain in patients who have undergone multi-level ACDF and thus correction of neck kyphosis can be related to improve postoperative neurological function recovery and on the other hand, cause removing axial neck pain after surgery, which can be controlled by correcting the moderate curvature of the neck [17]. Bai et al. [18] observed that postoperative axial pain will significantly become more prevalent if the surgical segment changes in its intervertebral height after ACDF by over 10%. However, in our study, intervertebral height changed much more than 10%, and severe axial pain correlated with postoperative disc height change was not observed. A similar result has been reported by Chang et al. [19] who evaluated the increase in intervertebral space by inserting a large graft material while performing ACDF to treat degenerative cervical disease. These authors claimed no correlation between intervertebral disc height change and the occurrence and severity of postoperative axial pain, which is consistent with our results. In a study by Cao et al [15], correlation analysis showed that the preoperative C2-C7 Cobb angle was significantly correlated with the severity of the postoperative axial pain. In addition, logistic regression analysis demonstrated that the preoperative C2-C7 Cobb angle was an independent predictor of postoperative axial pain. In other words, according to the results of this research, it is essential to correct the cervical lordosis angle in patients who are candidates for ACDF surgery. On the other hand, it is assumed that the compensatory mechanisms to relieve the axial pain of patients who are candidates for neck surgery cause their cervical alignment disorder, and by relieving the pain, these mechanisms are removed and the cervical alignment is corrected to some extent. Perhaps the significance of this relationship can be determined through the design of future studies with a larger sample size.
5. Conclusion
According to the results obtained from the present study, neck pain in candidates for ACDF surgery decreases after the surgical procedure. The study also indicates that the disruption of the cervical spine ligaments, which itself sets the stage for the occurrence of neck pain even after surgery, is significantly improved after ACDF surgery. Although a direct correlation was observed between pain reduction and the correction of the cervical lordosis angle after surgery existed, this correlation was not statistically significant.
In this study, it was demonstrated that the shorter the duration of symptoms, the more patients with severe pain sought medical attention. This correlation can be interpreted as suggesting that patients experiencing more severe pain tend to seek medical help earlier and are consequently referred for surgery sooner.
Furthermore, the results indicate that younger patients experience greater pain intensity. This may suggest that the chronic progression occurs more prominently in older individuals, leading to gradual adaptation to the conditions and subsequently a lesser perception of pain intensity.
Regarding the size of the cage between the vertebrae used, no significant relationship with the severity of neck pain after the surgery was observed.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered and the participants were informed in advance of the purpose of the study.
Funding
This paper was extracted from the thesis of Naghmeh Khoshsima, at Faculty of Medicine, Guilan University of Medical Science.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
References
Full Text: (1252 Views)
1. Introduction
Degenerative cervical myelopathy (DCM) is the most common cause of spinal cord weakness in adults due to various congenital or acquired causes leading to degeneration, hypertrophy, or calcification of the cervical spine’s intervertebral disc, ligaments, or bone structures [1]. These pathological processes cause narrowing of the cervical spinal canal, chronic compression of the spinal cord and neurological and functional disability [2]. Axial neck pain is commonly seen in patients with DCM defects, which is controlled by conservative measures in most cases [3], but neurosurgical measures are required in some patients. In some patients, this pain remains even after surgery needing more investigations to find the cause of the pain [4].
The importance of diagnosing underlying deformity in the sagittal alignment of the neck, such as abnormal C2 to C7 sagittal vertical axis or abnormal C2 to C7 Cobb angle has been shown in recent studies that neglecting these parameters can reduce the long-term quality of life of patients undergoing surgery [5, 6, 7]. Failure to repair these deformities can be one of the causes of debilitating pain in patients; however, some studies have also shown that excessive correction of these defects may also be the cause of axial neck pain in patients after surgery [8].
One of the common surgical methods in patients suffering from DCM is anterior cervical discectomy with fusion (ACDF) which is performed by removing the disc and posterior longitudinal ligament and placing a graft in the intervertebral space [9]. Some patients experience axial neck pain after ACDF surgery; which refers to the remaining pain after two months of surgery and can be felt in the neck, shoulder, or intrascapular space [6]. The appearance of this pain may refer to several factors, such as the severity of disc space distraction, the rate of lordosis angle of the neck before surgery, and also the duration of disease symptoms [10, 11]. In this study, we intended to assess the lordosis angle of the neck before and after the ACDF surgery and its relationship with axial neck pain changes before and after surgery. Confirmation of such a relationship provides a solution for the correction of this angle to prevent axial neck pain after surgery.
2. Materials and Methods
This longitudinal analytical study was performed on 60 consecutive male and female patients who were scheduled to undergo ACDF surgery due to neck disc or DCM and had axial neck pain before the operation who were operated in Poursina Hospital, Rasht, City, Iran since the beginning of the study. People with a history of rheumatoid arthritis or neurofibromatosis and patients operated on due to acute trauma were excluded from the study in addition to those who did not refer for post-operative examinations. The patients who did not have access to medical centers and communication devices after the first post-operative visit (on the first day after the operation) and had been discharged from the hospital were excluded too.
Once a patient was identified as suitable for the study, informed and voluntary consent was obtained, explaining to them that their names would not be disclosed to maintain privacy in the research. If the patient consented to participate, they were enrolled in the study.
Patients were evaluated at four visits before the surgery, the day after the surgery, 2 months after the surgery and 6 months after the surgery, as explained in sections 3-5. Necessary information was collected during these visits.
To analyze the collected data, changes in the C2-C7 Cobb angle before the surgery, the day after the surgery, 2 months and 6 months after the surgery were measured, as well as their pairwise comparisons. Visual analogue scale (VAS) scores were also assessed in the same sequence and manner. The correlation between changes in the C2-C7 Cobb angle and VAS scores of patients was then examined. Additionally, the relationship between age, gender, the size of the cervical collar used in patients and VAS scores along with Cobb angle changes was investigated.
After entering the study, the researcher collected the patient’s information, including name, phone number, and file number for further follow-up. Pre-operative investigations included recording information, such as age, gender, and the duration of the symptoms. The patients’ axial neck pain was determined using the VAS method and the patient was asked to rate pain severity in such a way that 0 indicates no pain and 10 indicates the most severe pain that can be described. Then, a simple lateral neck x-ray was taken in a position where all seven neck vertebrae were visible. According to the purpose of the research, the colleagues of the radiology unit were requested to perform an X-ray while standing so that the patient was in a weight-bearing position and the angles were calculated more accurately. To calculate the Cobb angle, if the patient’s graph was in the hospital’s picture archiving and communication system (PACS) system (where patient imaging is available on the hospital’s computer systems), the facilities built into the system were used to calculate the angle. If the imaging was printed, or not available in the hospital system, the Cobb angle was calculated by taking an image from it and importing the image into the Surgimap software.
Patients underwent surgery in the morning after hospitalization. Without knowing that the patient was the subject of research, the surgeon chose the size of the intervertebral cage based on his opinion and experience and based on the patient’s condition. The size of this cage was recorded in the patient’s file according to the usual procedure of the operating room. The day after the surgery, the patient was revisited in the ward and was again asked to determine his/her pain score based on the VAS scale. Also, the patient was sent to the radiology unit by closing the cervical collar to perform a simple lateral neck X-ray in a standing position and the X-ray was checked according to the described method. The patients were discharged on the day after the operation and were revisited two weeks, two months and six months later. In re-visits, according to the day after the operation, VAS was evaluated and an X-ray was taken for examination.
After data collection, the results were analyzed using SPSS software, version 22. This study reported descriptive statistics of qualitative variables using frequency and percentage and quantitative data using mean and standard deviation. A t-test was used to compare the results between groups. The chi-square test was used to compare qualitative variables. In this study, P<0.05 was considered as a significant level. The change in the quantitative parameters within six months was assessed using the repeated measure analysis of variance (ANOVA) test. The correct presentation of people’s data, use of reliable and new methods to get correct results, respect honesty and trustworthiness, respect honesty when analyzing and keeping the information of the people under investigation confidential, carefulness in the good use of funds and equipment were all the ethical principles of the study.
3. Results
This research was conducted to investigate the correlation between changes in cervical Cobb angle and neck axial pain before and after surgery in patients undergoing cervical discectomy at Poursina Hospital. After collecting the data, relevant analyses were conducted using SPSS software, version 22. Table 1 presents the frequency distribution of the samples using descriptive statistics.

Based on the results presented in Table 1, most research samples (56.67%) were male, and most of them (41.7%) fell within the age range of 40 to 50 years, with an average age of 47.10±8.44 years. A significant portion (66.7%) experienced symptoms for less than six months, with an average duration of symptoms per month equal to 4.62±4.49. The gauge size in most samples was 6, accounting for 36.7%, followed by 5 with 30%. Before surgery, the patients suffered from significant axial neck pain with a mean pain score of 7.47±2.02, but after surgery, patients experienced a downward trend of changes in pain score as the mean pain score of 0.92±1.46 at two weeks, 1.31±1.63 at two months and 1.32±1.64 at six months after operation. The repeated measure ANOVA test showed a significant reduction in pain score within follow-up time (P<0.001). Assessing the changes in pain score in men and women (Table 2), showed no difference between the two genders in different time points.
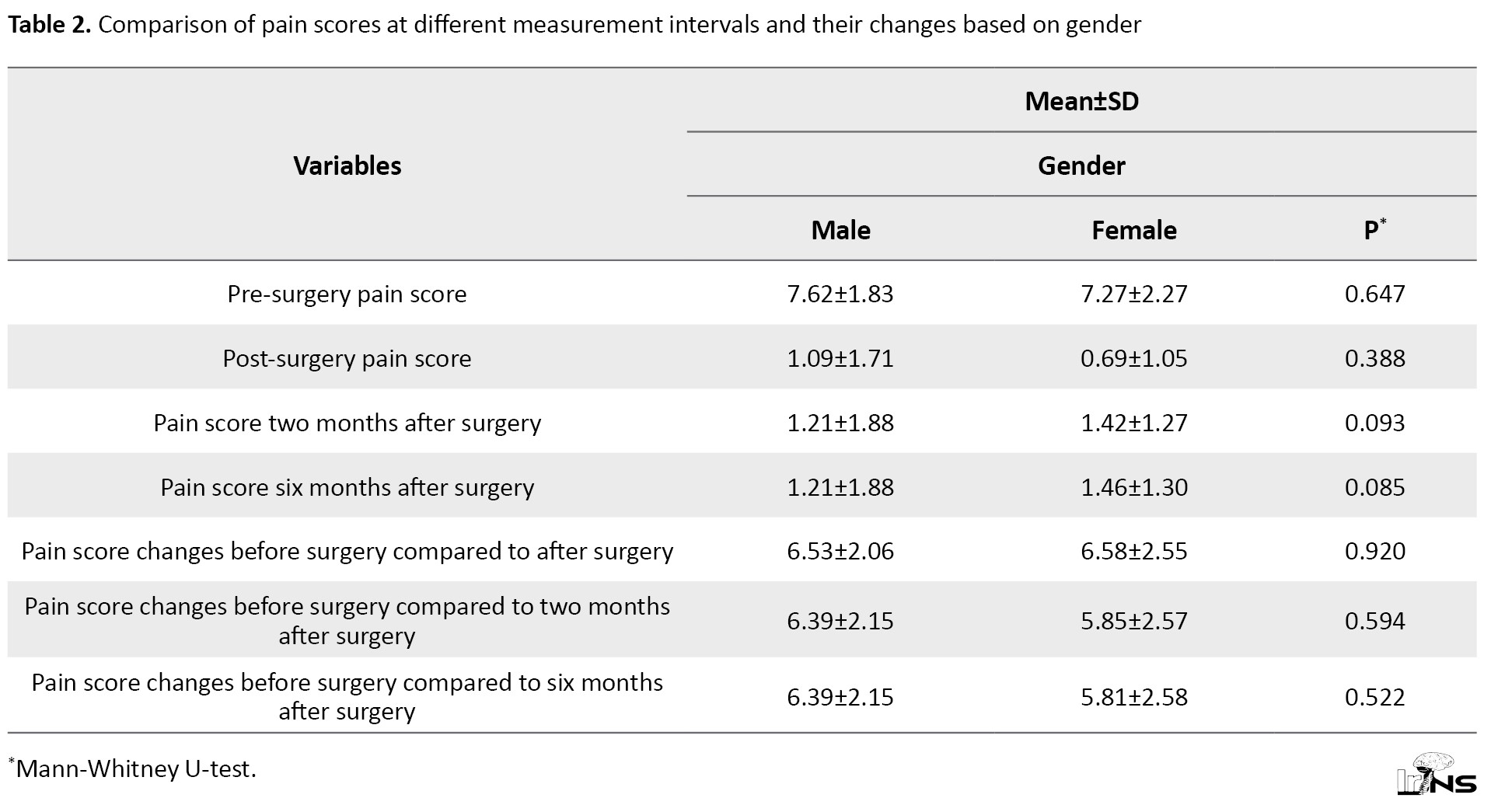
According to the results presented in Table 2, no statistically significant difference was observed in pain scores measured at different intervals and their changes between males and females.
Regarding the mean pain score according to patients’ age (Table 3), an adverse relationship was found between pain severity and age before surgery (r=-0.340, P=0.008).
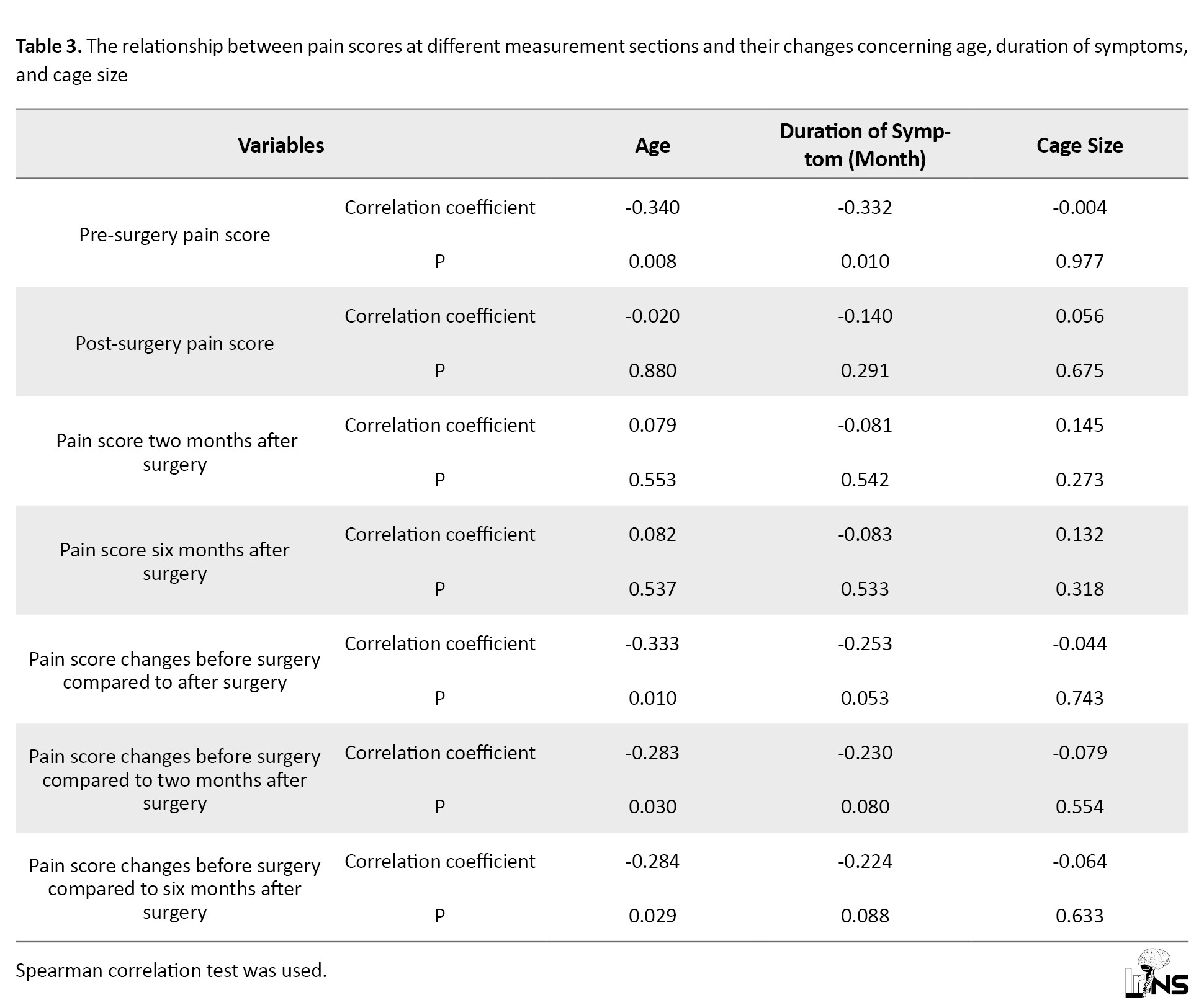
An adverse relationship was also revealed between pain score before surgery and duration of symptoms (r=-0.332, P=0.010). However, no relationship was observed between pain score at different time points and the size of the cage.
Based on the results in Table 3, a statistically significant and inverse correlation was observed between pre-surgery pain scores and age as well as the duration of symptoms (r=-0.332, P=0.010) and (r=-0.340, P=0.008). In other words, as age and the duration of symptoms increased, the pain scores decreased. Therefore, in the elderly population, pre-surgery pain scores were lower. Additionally, patients with a longer duration of symptoms experienced less pre-surgery pain. The changes in pre-surgery pain scores compared to post-surgery, two months post-surgery, and six months post-surgery also exhibited a statistically significant inverse correlation with age.
Following the description of sample frequencies, the mean pain scores before and after surgery, two months after surgery, and six months after surgery were calculated using the Friedman test. The results of the test which showed significant pain difference before and after the surgery (P<0.001), are presented in Tables 4 and Figure 1.

Degenerative cervical myelopathy (DCM) is the most common cause of spinal cord weakness in adults due to various congenital or acquired causes leading to degeneration, hypertrophy, or calcification of the cervical spine’s intervertebral disc, ligaments, or bone structures [1]. These pathological processes cause narrowing of the cervical spinal canal, chronic compression of the spinal cord and neurological and functional disability [2]. Axial neck pain is commonly seen in patients with DCM defects, which is controlled by conservative measures in most cases [3], but neurosurgical measures are required in some patients. In some patients, this pain remains even after surgery needing more investigations to find the cause of the pain [4].
The importance of diagnosing underlying deformity in the sagittal alignment of the neck, such as abnormal C2 to C7 sagittal vertical axis or abnormal C2 to C7 Cobb angle has been shown in recent studies that neglecting these parameters can reduce the long-term quality of life of patients undergoing surgery [5, 6, 7]. Failure to repair these deformities can be one of the causes of debilitating pain in patients; however, some studies have also shown that excessive correction of these defects may also be the cause of axial neck pain in patients after surgery [8].
One of the common surgical methods in patients suffering from DCM is anterior cervical discectomy with fusion (ACDF) which is performed by removing the disc and posterior longitudinal ligament and placing a graft in the intervertebral space [9]. Some patients experience axial neck pain after ACDF surgery; which refers to the remaining pain after two months of surgery and can be felt in the neck, shoulder, or intrascapular space [6]. The appearance of this pain may refer to several factors, such as the severity of disc space distraction, the rate of lordosis angle of the neck before surgery, and also the duration of disease symptoms [10, 11]. In this study, we intended to assess the lordosis angle of the neck before and after the ACDF surgery and its relationship with axial neck pain changes before and after surgery. Confirmation of such a relationship provides a solution for the correction of this angle to prevent axial neck pain after surgery.
2. Materials and Methods
This longitudinal analytical study was performed on 60 consecutive male and female patients who were scheduled to undergo ACDF surgery due to neck disc or DCM and had axial neck pain before the operation who were operated in Poursina Hospital, Rasht, City, Iran since the beginning of the study. People with a history of rheumatoid arthritis or neurofibromatosis and patients operated on due to acute trauma were excluded from the study in addition to those who did not refer for post-operative examinations. The patients who did not have access to medical centers and communication devices after the first post-operative visit (on the first day after the operation) and had been discharged from the hospital were excluded too.
Once a patient was identified as suitable for the study, informed and voluntary consent was obtained, explaining to them that their names would not be disclosed to maintain privacy in the research. If the patient consented to participate, they were enrolled in the study.
Patients were evaluated at four visits before the surgery, the day after the surgery, 2 months after the surgery and 6 months after the surgery, as explained in sections 3-5. Necessary information was collected during these visits.
To analyze the collected data, changes in the C2-C7 Cobb angle before the surgery, the day after the surgery, 2 months and 6 months after the surgery were measured, as well as their pairwise comparisons. Visual analogue scale (VAS) scores were also assessed in the same sequence and manner. The correlation between changes in the C2-C7 Cobb angle and VAS scores of patients was then examined. Additionally, the relationship between age, gender, the size of the cervical collar used in patients and VAS scores along with Cobb angle changes was investigated.
After entering the study, the researcher collected the patient’s information, including name, phone number, and file number for further follow-up. Pre-operative investigations included recording information, such as age, gender, and the duration of the symptoms. The patients’ axial neck pain was determined using the VAS method and the patient was asked to rate pain severity in such a way that 0 indicates no pain and 10 indicates the most severe pain that can be described. Then, a simple lateral neck x-ray was taken in a position where all seven neck vertebrae were visible. According to the purpose of the research, the colleagues of the radiology unit were requested to perform an X-ray while standing so that the patient was in a weight-bearing position and the angles were calculated more accurately. To calculate the Cobb angle, if the patient’s graph was in the hospital’s picture archiving and communication system (PACS) system (where patient imaging is available on the hospital’s computer systems), the facilities built into the system were used to calculate the angle. If the imaging was printed, or not available in the hospital system, the Cobb angle was calculated by taking an image from it and importing the image into the Surgimap software.
Patients underwent surgery in the morning after hospitalization. Without knowing that the patient was the subject of research, the surgeon chose the size of the intervertebral cage based on his opinion and experience and based on the patient’s condition. The size of this cage was recorded in the patient’s file according to the usual procedure of the operating room. The day after the surgery, the patient was revisited in the ward and was again asked to determine his/her pain score based on the VAS scale. Also, the patient was sent to the radiology unit by closing the cervical collar to perform a simple lateral neck X-ray in a standing position and the X-ray was checked according to the described method. The patients were discharged on the day after the operation and were revisited two weeks, two months and six months later. In re-visits, according to the day after the operation, VAS was evaluated and an X-ray was taken for examination.
After data collection, the results were analyzed using SPSS software, version 22. This study reported descriptive statistics of qualitative variables using frequency and percentage and quantitative data using mean and standard deviation. A t-test was used to compare the results between groups. The chi-square test was used to compare qualitative variables. In this study, P<0.05 was considered as a significant level. The change in the quantitative parameters within six months was assessed using the repeated measure analysis of variance (ANOVA) test. The correct presentation of people’s data, use of reliable and new methods to get correct results, respect honesty and trustworthiness, respect honesty when analyzing and keeping the information of the people under investigation confidential, carefulness in the good use of funds and equipment were all the ethical principles of the study.
3. Results
This research was conducted to investigate the correlation between changes in cervical Cobb angle and neck axial pain before and after surgery in patients undergoing cervical discectomy at Poursina Hospital. After collecting the data, relevant analyses were conducted using SPSS software, version 22. Table 1 presents the frequency distribution of the samples using descriptive statistics.

Based on the results presented in Table 1, most research samples (56.67%) were male, and most of them (41.7%) fell within the age range of 40 to 50 years, with an average age of 47.10±8.44 years. A significant portion (66.7%) experienced symptoms for less than six months, with an average duration of symptoms per month equal to 4.62±4.49. The gauge size in most samples was 6, accounting for 36.7%, followed by 5 with 30%. Before surgery, the patients suffered from significant axial neck pain with a mean pain score of 7.47±2.02, but after surgery, patients experienced a downward trend of changes in pain score as the mean pain score of 0.92±1.46 at two weeks, 1.31±1.63 at two months and 1.32±1.64 at six months after operation. The repeated measure ANOVA test showed a significant reduction in pain score within follow-up time (P<0.001). Assessing the changes in pain score in men and women (Table 2), showed no difference between the two genders in different time points.

According to the results presented in Table 2, no statistically significant difference was observed in pain scores measured at different intervals and their changes between males and females.
Regarding the mean pain score according to patients’ age (Table 3), an adverse relationship was found between pain severity and age before surgery (r=-0.340, P=0.008).

An adverse relationship was also revealed between pain score before surgery and duration of symptoms (r=-0.332, P=0.010). However, no relationship was observed between pain score at different time points and the size of the cage.
Based on the results in Table 3, a statistically significant and inverse correlation was observed between pre-surgery pain scores and age as well as the duration of symptoms (r=-0.332, P=0.010) and (r=-0.340, P=0.008). In other words, as age and the duration of symptoms increased, the pain scores decreased. Therefore, in the elderly population, pre-surgery pain scores were lower. Additionally, patients with a longer duration of symptoms experienced less pre-surgery pain. The changes in pre-surgery pain scores compared to post-surgery, two months post-surgery, and six months post-surgery also exhibited a statistically significant inverse correlation with age.
Following the description of sample frequencies, the mean pain scores before and after surgery, two months after surgery, and six months after surgery were calculated using the Friedman test. The results of the test which showed significant pain difference before and after the surgery (P<0.001), are presented in Tables 4 and Figure 1.

As mentioned, a repeated measure of ANOVA (Table 5) was used to check the trend of changes in pain scores at different pre-surgery, and post-surgery intervals, two months after surgery and six months after surgery.

According to this test analysis, the trend of the changes in Cobb angle after surgery was significant (P<0.001). This trend of changes has been summarized in Table 5.
Furthermore, using the multivariate linear regression modeling with the presence of baseline parameters and the changes in the Cobb angle (Table 6), the relationship between the pain score and Cobb angle remained insignificant (P=0.387).
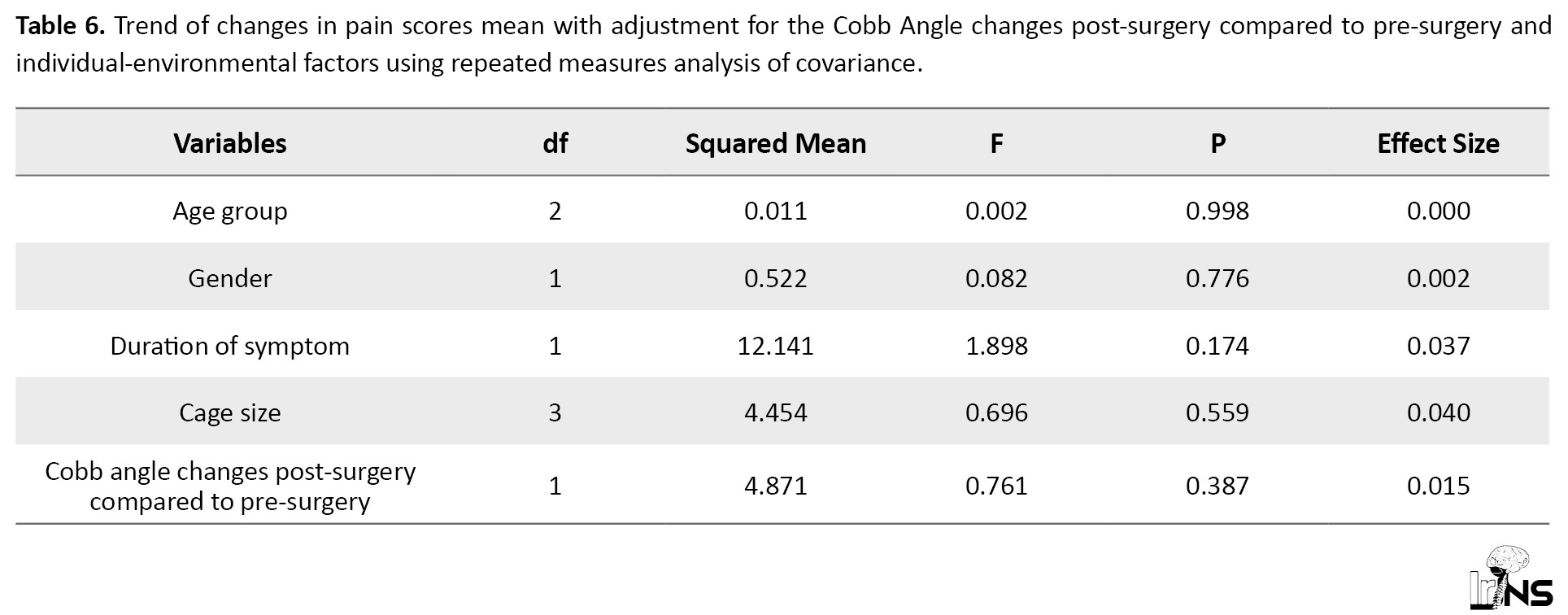
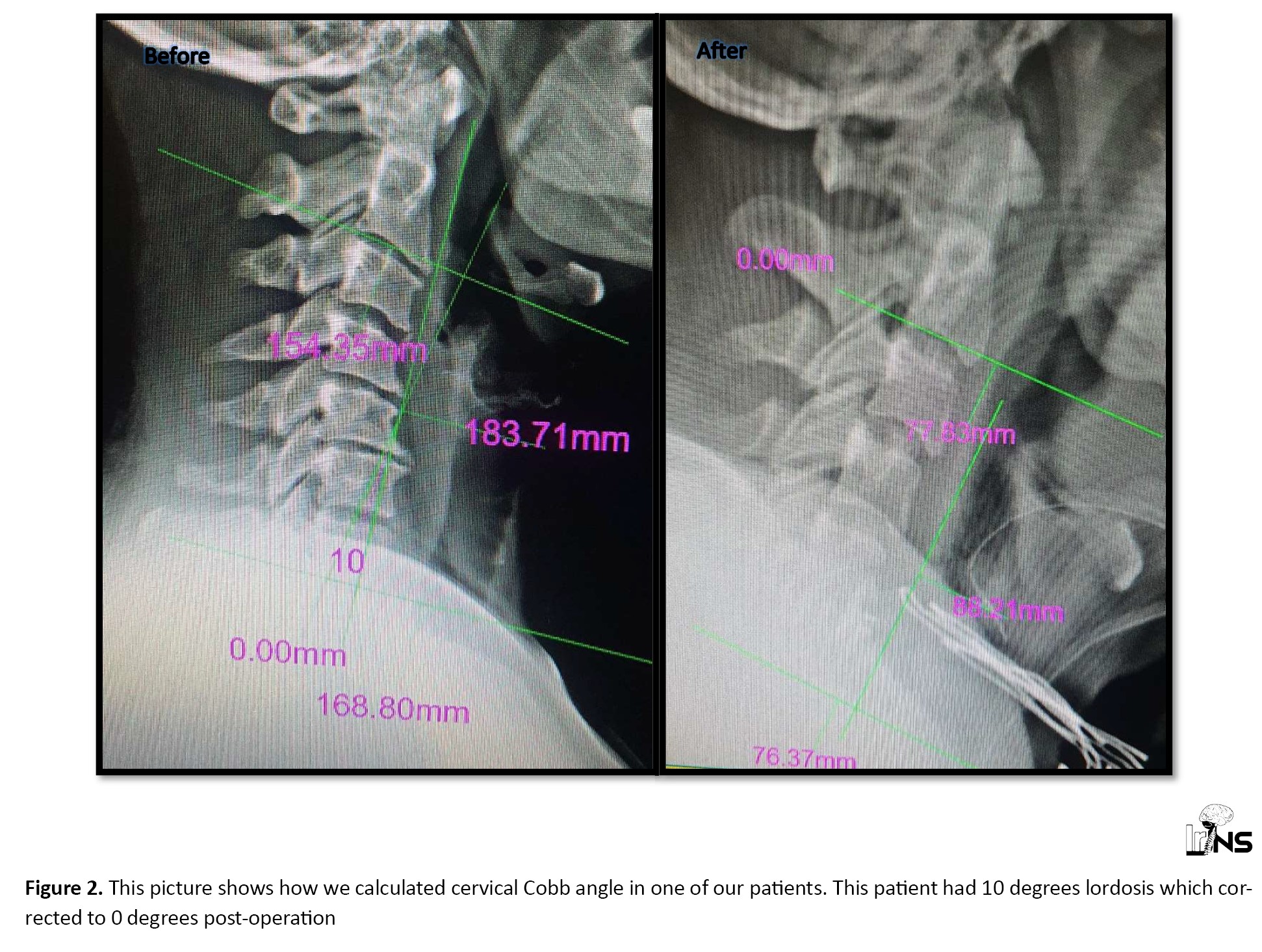
Concerning the changes in Cobb angle after surgery, significant improvements were revealed in this parameter after the operation that the mean value of this angle at two weeks, two months, and six months after surgery was significantly lower than that observed before surgery. As indicated in Table 6, no significant relationship was observed between axial neck pain score and Cobb angle before as well as at different time points after surgery.
Based on the results presented in Table 6, using one-way ANOVA for repeated measure, it was observed that none of the variables, including age, gender, duration of symptoms, cage size and Cobb angle changes had a statistically significant correlation with the trend of pain score changes. Figure 2 shows how the C2-C7 cobb angle calculation was performed.

According to this test analysis, the trend of the changes in Cobb angle after surgery was significant (P<0.001). This trend of changes has been summarized in Table 5.
Furthermore, using the multivariate linear regression modeling with the presence of baseline parameters and the changes in the Cobb angle (Table 6), the relationship between the pain score and Cobb angle remained insignificant (P=0.387).

Concerning the changes in Cobb angle after surgery, significant improvements were revealed in this parameter after the operation that the mean value of this angle at two weeks, two months, and six months after surgery was significantly lower than that observed before surgery. As indicated in Table 6, no significant relationship was observed between axial neck pain score and Cobb angle before as well as at different time points after surgery.
Based on the results presented in Table 6, using one-way ANOVA for repeated measure, it was observed that none of the variables, including age, gender, duration of symptoms, cage size and Cobb angle changes had a statistically significant correlation with the trend of pain score changes. Figure 2 shows how the C2-C7 cobb angle calculation was performed.
4. Discussion
Considering that degenerative neck diseases have a high prevalence and ACDF surgery is one of the common surgeries in neurosurgery patients, and also considering that sometimes patients still mention axial neck pain after surgery, it is felt necessary to conduct some studies for finding possible causes of this pain and to provide solutions to remove it. Therefore, in this research, an attempt was made to take a step in this direction by examining the Cobb angle before and after surgery and its correlation with axial neck pain following operation.
One limitation encountered in this study was the usual practice of obtaining pre- and post-surgery lateral cervical X-rays with patients lying down, given pain relief and immobility with a hard collar after surgery. To address this issue, requests were made to the radiology unit for standing X-rays in weight-bearing conditions to enhance the accuracy of C2-C7 Cobb angle calculation.
Another challenge was that some patients had no access to communication tools and medical facilities for the third and fourth visits, after entering the study and providing their information at the pre-surgery and immediate post-surgery visits, leading to their exclusion from subsequent comparisons within the study population.
Furthermore, some patients had printed neck X-rays or no access to the hospital’s PACS system, making it difficult to import the image into the Surgimap software for Cobb angle calculation.
The first result of this research shows that the average pain score after the operation has decreased significantly compared to before the operation and this difference was statistically significant. This difference was evident until the second and sixth months after the operation. This result is also confirmed in other research in this field that ACDF is associated with a clear reduction of axial neck pain in patients who have undergone surgery, especially for the treatment of myelopathy or radiculopathy. In a recent meta-analysis by Harrop et al. [12], patients with neck pain predominant had a greater reduction in neck pain after surgical fusion with a change from a baseline of 53.4%. In another study by Riew et al. [13], a mean improvement of the pain of at least 50% was observed approximately 4 years following surgery. In their study, functional outcomes improved between 32% and 52% from baseline. In another systematic review and meta-analysis by Oitment et al. [14], the individual neck pain mean differences were reduced at different time points after surgery from 6 weeks to 48 months of follow-up. Therefore, it can be said that for the management of patients’ axial neck pain due to DCM, ACDF surgery can be an option of choice for these patients.
As another critical result, the mean absolute value of the Cobb angle increased after surgery compared to before surgery, and this difference was statistically significant. This increase was evident until the second and sixth months after the operation. Also, the results of this study show that the average changes in the Cobb angle of each measurement period after the operation (two to six months after the operation) were statistically different from before the operation and this trend was decreasing. However, we found no relationship between neck pain with Cobb angle in different time points, which could potentially be influenced by our small sample size. However, in the investigation of the possible influence of other background indicators, such as age, sex, cage size and duration of disease symptoms, the relationship between pain and angle changes remained non-significant. In an article published by Yuan Cao et al, 144 zero-profile ACDF patients were examined, of which 48 had axial neck pain after surgery. The patients were followed up for one year and they finally concluded that the C2-C7 Cobb angle before surgery is a risk factor for severe axial pain after surgery in zero-profile ACDF patients [15]. Similarly, in a retrospective cohort study by Canseco et al. 308 patients who underwent ACDF at one to three levels were examined, and found that patients in whom the C2-C7 Cobb angle was corrected to a neutral or lordotic position had more axial neck improvement as compared to patients with the kyphotic state [16]. In Liu et al. study on 88 patients who were followed for one year, it was found that preoperative neck pain severity and kyphosis status can predict the severity of postoperative neck pain in patients who have undergone multi-level ACDF and thus correction of neck kyphosis can be related to improve postoperative neurological function recovery and on the other hand, cause removing axial neck pain after surgery, which can be controlled by correcting the moderate curvature of the neck [17]. Bai et al. [18] observed that postoperative axial pain will significantly become more prevalent if the surgical segment changes in its intervertebral height after ACDF by over 10%. However, in our study, intervertebral height changed much more than 10%, and severe axial pain correlated with postoperative disc height change was not observed. A similar result has been reported by Chang et al. [19] who evaluated the increase in intervertebral space by inserting a large graft material while performing ACDF to treat degenerative cervical disease. These authors claimed no correlation between intervertebral disc height change and the occurrence and severity of postoperative axial pain, which is consistent with our results. In a study by Cao et al [15], correlation analysis showed that the preoperative C2-C7 Cobb angle was significantly correlated with the severity of the postoperative axial pain. In addition, logistic regression analysis demonstrated that the preoperative C2-C7 Cobb angle was an independent predictor of postoperative axial pain. In other words, according to the results of this research, it is essential to correct the cervical lordosis angle in patients who are candidates for ACDF surgery. On the other hand, it is assumed that the compensatory mechanisms to relieve the axial pain of patients who are candidates for neck surgery cause their cervical alignment disorder, and by relieving the pain, these mechanisms are removed and the cervical alignment is corrected to some extent. Perhaps the significance of this relationship can be determined through the design of future studies with a larger sample size.
5. Conclusion
According to the results obtained from the present study, neck pain in candidates for ACDF surgery decreases after the surgical procedure. The study also indicates that the disruption of the cervical spine ligaments, which itself sets the stage for the occurrence of neck pain even after surgery, is significantly improved after ACDF surgery. Although a direct correlation was observed between pain reduction and the correction of the cervical lordosis angle after surgery existed, this correlation was not statistically significant.
In this study, it was demonstrated that the shorter the duration of symptoms, the more patients with severe pain sought medical attention. This correlation can be interpreted as suggesting that patients experiencing more severe pain tend to seek medical help earlier and are consequently referred for surgery sooner.
Furthermore, the results indicate that younger patients experience greater pain intensity. This may suggest that the chronic progression occurs more prominently in older individuals, leading to gradual adaptation to the conditions and subsequently a lesser perception of pain intensity.
Regarding the size of the cage between the vertebrae used, no significant relationship with the severity of neck pain after the surgery was observed.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered and the participants were informed in advance of the purpose of the study.
Funding
This paper was extracted from the thesis of Naghmeh Khoshsima, at Faculty of Medicine, Guilan University of Medical Science.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
References
- Davies BM, Mowforth OD, Smith EK, Kotter MR. Degenerative cervical myelopathy. BMJ. 2018; 360:k186. [DOI:10.1136/bmj.k186] [PMID] [PMCID]
- Williams J, D'Amore P, Redlich N, Darlow M, Suwak P, Sarkovich S, et al. Degenerative cervical myelopathy: Evaluation and management. The Orthopedic Clinics of North America. 2022; 53(4):509-21. [DOI:10.1016/j.ocl.2022.05.007] [PMID]
- Badhiwala JH, Ahuja CS, Akbar MA, Witiw CD, Nassiri F, Furlan JC, et al. Degenerative cervical myelopathy-update and future directions. Nature Reviews. Neurology. 2020; 16(2):108-24. [DOI:10.1038/s41582-019-0303-0] [PMID]
- Chen R, Liu J, Zhao Y, Diao Y, Chen X, Pan S, et al. Predictive value of preoperative short form-36 survey scale for postoperative axial neck pain in patients with degenerative cervical myelopathy. Global Spine Journal. 2023; 21925682231200136. [DOI:10.1177/21925682231200136] [PMID]
- Liu T, Tian S, Zhang J, He M, Deng L, Ding W, et al. Comparison of cervical sagittal parameters among patients with neck pain and patients with cervical spondylotic radiculopathy and cervical spondylotic myelopathy. Orthopaedic Surgery. 2024; 16(2):329-36. [DOI:10.1111/os.13951] [PMID] [PMCID]
- Zhao HH, Xu HW, Wang SJ, Hu T, Wu DS. Anterior cervical discectomy and fusion with a zero-profile VA spacer device: A clinical and radiological study with two-year follow-up. Journal of Orthopaedic Surgery and Research. 2024; 19(1):51. [DOI:10.1186/s13018-024-04539-9] [PMID] [PMCID]
- Chan AK, Shaffrey CI, Gottfried ON, Park C, Than KD, Bisson EF, et al. Cervical spondylotic myelopathy with severe axial neck pain: Is anterior or posterior approach better? Journal of Neurosurgery. Spine. 2022; 38(1):42-55. [DOI:10.3171/2022.6.SPINE22110] [PMID]
- Goh GS, Yue WM, Guo CM, Tan SB, Chen JL. Does the predominant pain location influence functional outcomes, satisfaction and return to work after anterior cervical discectomy and fusion for cervical radiculopathy? Spine. 2021; 46(10):E568-75. [DOI:10.1097/BRS.0000000000003855] [PMID]
- Bunmaprasert T, Keeratiruangrong J, Lee SH, Sugandhavesa N, Liawrungrueang W. Cervical sagittal parameters in degenerative cervical spondylolisthesis versus degenerative cervical kyphosis with myeloradiculopathy treated by anterior cervical discectomy and fusion. Journal of Spine Surgery. 2024; 10(1):109-19. [DOI:10.21037/jss-23-107] [PMID] [PMCID]
- Patel MR, Jacob KC, Shah VP, Prabhu MC, Pawlowski H, Vanjani NN, et al. Influence of predominant neck versus arm pain on anterior cervical discectomy and fusion outcomes: A follow-up study. World Neurosurgery. 2022; 160:e288-95. [DOI:10.1016/j.wneu.2022.01.001] [PMID]
- Massel DH, Mayo BC, Bohl DD, Narain AS, Hijji FY, Fineberg SJ, et al. Improvements in neck and arm pain following an anterior cervical discectomy and fusion. Spine. 2017; 42(14):E825-32. [DOI:10.1097/BRS.0000000000001979] [PMID]
- Harrop JS, Gonzalez GA, Qasba RK, Porto G, Wainwright JV, Thalheimer S, et al. Does axial cervical pain improve with surgical fusion? A meta-analysis. Journal of Neurosurgery. Spine. 2023; 39(3):345-54. [DOI:10.3171/2023.4.SPINE23185] [PMID]
- Riew KD, Ecker E, Dettori JR. Anterior cervical discectomy and fusion for the management of axial neck pain in the absence of radiculopathy or myelopathy. Evidence-Based Spine-Care Journal. 2010; 1(3):45-50. [DOI:10.1055/s-0030-1267067] [PMID] [PMCID]
- Oitment C, Watson T, Lam V, Aref M, Koziarz A, Kachur E, Badhiwala JH, et al. The role of anterior cervical discectomy and fusion on relieving axial neck pain in patients with single-level disease: A systematic review and meta-analysis. Global Spine Journal. 2020; 10(3):312-23. [DOI:10.1177/2192568219837923] [PMID] [PMCID]
- Cao Y, Xu C, Sun B, Cui C, Zhang K, Wu H, et al. Preoperative cervical cobb angle is a risk factor for postoperative axial neck pain after anterior cervical discectomy and fusion with zero-profile interbody. Orthopaedic Surgery. 2022; 14(12):3225-32. [DOI:10.1111/os.13552] [PMID] [PMCID]
- Canseco JA, Karamian BA, Patel PD, Markowitz M, Lee JK, Kurd MF, et al. Perioperative chanage in cervical lordosis and health-related quality-of-life outcomes. International Journal of Spine Surgery. 2022; 16(6):960-8. [DOI:10.14444/8325] [PMID] [PMCID]
- Liu S, Yang DL, Zhao RY, Yang SD, Ma L, Wang H, et al. Prevalence and risk factors of axial neck pain in patients undergoing multilevel anterior cervical decompression with fusion surgery. Journal of Orthopaedic Surgery and Research. 2019; 14(1):94. [DOI:10.1186/s13018-019-1132-y] [PMID] [PMCID]
- Bai J, Zhang X, Zhang D, Ding W, Shen Y, Zhang W, et al. Impact of over distraction on occurrence of axial symptom after anterior cervical discectomy and fusion. International Journal of Clinical and Experimental Medicine. 2015; 8(10):19746-56. [PMID] [PMCID]
- Chang H, Baek DH, Choi BW. The relationship between increased intervertebral disc height and development of postoperative axial neck pain after anterior cervical fusion. Journal of Korean Neurosurgical Society. 2014; 55(6):343-7. [DOI:10.3340/jkns.2014.55.6.343] [PMID] [PMCID]
Send email to the article author
| Rights and Permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |