Tue, Jul 8, 2025
Volume 5, Issue 3 And 4 (Summer & Autumn 2019)
Iran J Neurosurg 2019, 5(3 And 4): 125-132 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Leon B, Olivier Brice N, Sinclair Brice K B, Hugues Brieux E M. Tandem Spinal Stenosis at the Brazzaville Academic Hospital. Iran J Neurosurg 2019; 5 (3 and 4) :125-132
URL: http://irjns.org/article-1-175-en.html
URL: http://irjns.org/article-1-175-en.html
Boukassa Leon *1 

 , Ngackosso Olivier Brice2
, Ngackosso Olivier Brice2 

 , Kinata Bambino Sinclair Brice2
, Kinata Bambino Sinclair Brice2 

 , Ekouele Mbaki Hugues Brieux3
, Ekouele Mbaki Hugues Brieux3 




 , Ngackosso Olivier Brice2
, Ngackosso Olivier Brice2 

 , Kinata Bambino Sinclair Brice2
, Kinata Bambino Sinclair Brice2 

 , Ekouele Mbaki Hugues Brieux3
, Ekouele Mbaki Hugues Brieux3 


1- Marien Ngouabi University and Brazzaville Academic Hospital, Brazzaville, Republic of the Congo , lboukassalouf
2- Brazzaville Academic Hospital, Brazzaville, Republic of the Congo
3- Marien Ngouabi University and Brazzaville Academic Hospital, Brazzaville, Republic of the Congo
2- Brazzaville Academic Hospital, Brazzaville, Republic of the Congo
3- Marien Ngouabi University and Brazzaville Academic Hospital, Brazzaville, Republic of the Congo
Keywords: Tandem Spinal Stenosis (TSS), Simultaneous cervico-lumbar
stenosis, Simultaneous
thoraco-lumbar stenosis, Simultaneous cervico-thoracic
stenosis, Spine surgery
Full Text [PDF 683 kb]
(1379 Downloads)
| Abstract (HTML) (7110 Views)
Full Text: (5844 Views)
1. Introduction
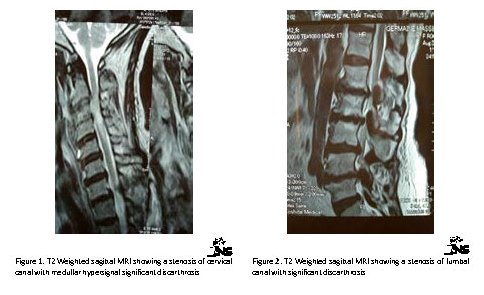
andem Spinal Stenosis (TSS) can be defined as simultaneous stenosis of two distinct spinal (cervical, thoracic and lumbar) areas [1]. The prevalence of the condition has been reported as 28% of patients with intermittent neurological claudication [2]. It is revealed according to Dagi [3] by the symptomatic triad. This is made up of intermittent neurogenic claudication, gait disturbances and signs of myelopathy and mixed polyradiculopathy of the extremities of thoracic and pelvic limbs. Magnetic resonance imaging, a morphological examination of choice presently, makes it possible to determine the type of tandem (Figures 1, 2). The treatment, among other surgical techniques, remains controversial. We reported the diagnostic and therapeutic strategies used for a group of patients at the Brazzaville Academic Hospital.
2. Methods and Materials/Patients
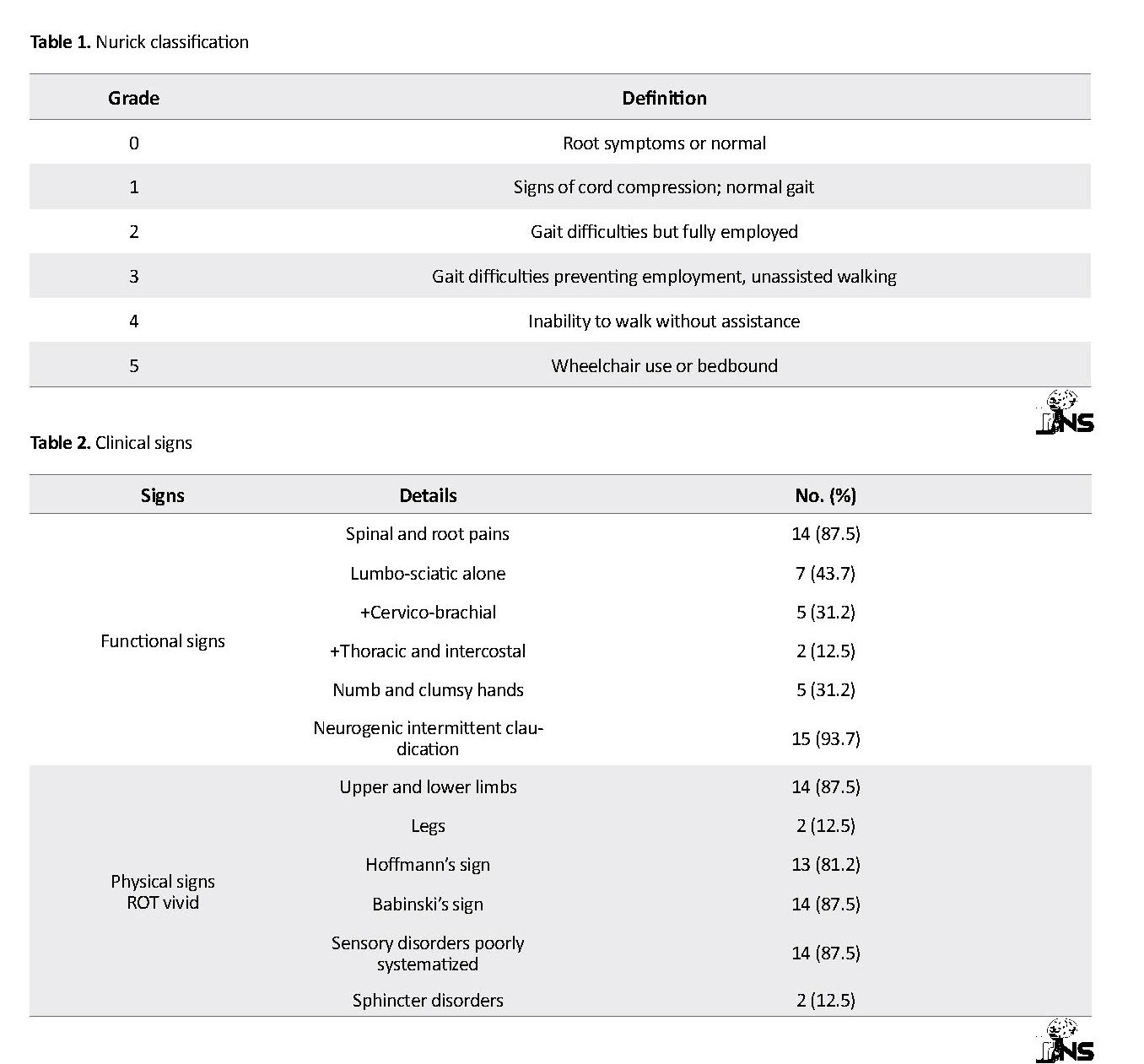
The study was conducted in the Neurosurgery Unit of the Brazzaville Academic Hospital Multipurpose Surgery Department, over a 10-year period (from June 2009 to May 2019). We identified 16 files. These were patients followed for at least two degenerative conditions in at least two separate spinal segments. In addition to demographic data, we analyzed clinical, paraclinical, therapeutic and evolutionary parameters. The clinical parameters were, among others, the duration of evolution of the signs and especially the repercussion of these signs on the autonomy of the patients. For the appreciation of this autonomy, Nurick classification by extrapolation has been employed (Table 1). Morphological data including the identification of different tandems and the number of disco-vertebral lesions per spinal segment were collected. Regarding the therapeutic parameters, it was mainly about the surgical planning with its mode (surgery in one or two stages), its order (cervico-thoraco-lumbar or not), its duration of realization and, the blood losses during this surgery. Lastly, the evolutionary parameters were evaluated by comparing Nurick’s pre- and postoperative grades. The transition from a patient with a higher Nurick grade to a lower stage is considered an improvement. The information obtained about spinal stenosis in tandem at the Brazzaville Academic hospital was recorded on an Excel sheet of Microsoft Office 2010.
3. Results
Over a period of 10 years (from June 2009 to May 2019), the data of 1664 patients had been recorded for degenerative pathology of the spine. TSS with 16 cases accounted for 0.96% of cases, or 1.6 cases per year. The sex ratio was 1.3. The average age of spinal stenosis in tandem at the Brazzaville Academic hospital was 57 years (41 and 71 years). The symptoms evolved for 17.6 months on average. The clinical signs observed in these patients are contained in the Table 2. According to Nurick’s classification, three patients were in stage 1, seven in stage 2, four in stage 3, and finally two in stage 4.
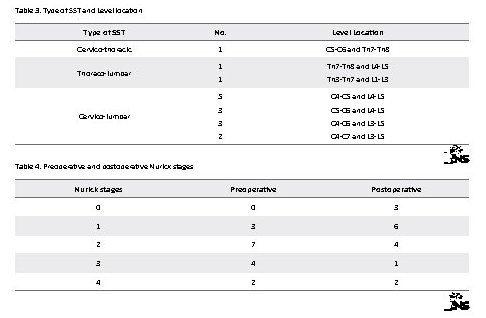
Medical imaging was represented by Saccoradiculography associated with Myeloscanner in 5 patients and cervico-thoraco-lumbar MRI in 11 patients. The results of this morphological assessment are recorded in the Table 3.
andem Spinal Stenosis (TSS) can be defined as simultaneous stenosis of two distinct spinal (cervical, thoracic and lumbar) areas [1]. The prevalence of the condition has been reported as 28% of patients with intermittent neurological claudication [2]. It is revealed according to Dagi [3] by the symptomatic triad. This is made up of intermittent neurogenic claudication, gait disturbances and signs of myelopathy and mixed polyradiculopathy of the extremities of thoracic and pelvic limbs. Magnetic resonance imaging, a morphological examination of choice presently, makes it possible to determine the type of tandem (Figures 1, 2). The treatment, among other surgical techniques, remains controversial. We reported the diagnostic and therapeutic strategies used for a group of patients at the Brazzaville Academic Hospital.
2. Methods and Materials/Patients
The study was conducted in the Neurosurgery Unit of the Brazzaville Academic Hospital Multipurpose Surgery Department, over a 10-year period (from June 2009 to May 2019). We identified 16 files. These were patients followed for at least two degenerative conditions in at least two separate spinal segments. In addition to demographic data, we analyzed clinical, paraclinical, therapeutic and evolutionary parameters. The clinical parameters were, among others, the duration of evolution of the signs and especially the repercussion of these signs on the autonomy of the patients. For the appreciation of this autonomy, Nurick classification by extrapolation has been employed (Table 1). Morphological data including the identification of different tandems and the number of disco-vertebral lesions per spinal segment were collected. Regarding the therapeutic parameters, it was mainly about the surgical planning with its mode (surgery in one or two stages), its order (cervico-thoraco-lumbar or not), its duration of realization and, the blood losses during this surgery. Lastly, the evolutionary parameters were evaluated by comparing Nurick’s pre- and postoperative grades. The transition from a patient with a higher Nurick grade to a lower stage is considered an improvement. The information obtained about spinal stenosis in tandem at the Brazzaville Academic hospital was recorded on an Excel sheet of Microsoft Office 2010.
3. Results
Over a period of 10 years (from June 2009 to May 2019), the data of 1664 patients had been recorded for degenerative pathology of the spine. TSS with 16 cases accounted for 0.96% of cases, or 1.6 cases per year. The sex ratio was 1.3. The average age of spinal stenosis in tandem at the Brazzaville Academic hospital was 57 years (41 and 71 years). The symptoms evolved for 17.6 months on average. The clinical signs observed in these patients are contained in the Table 2. According to Nurick’s classification, three patients were in stage 1, seven in stage 2, four in stage 3, and finally two in stage 4.
Medical imaging was represented by Saccoradiculography associated with Myeloscanner in 5 patients and cervico-thoraco-lumbar MRI in 11 patients. The results of this morphological assessment are recorded in the Table 3.
Two modes of Surgery have been used: surgery in one or two operating stages. Single stage surgery was performed in 2 patients. The surgical team was the same and involved a cervico-lumbar and thoraco-lumbar combination. For the other 14 cases, it was done in two stages. The average time interval between the two interventions was three months with extremes of 2-7 months. These were laminectomies with or without a vertebral fusion device, in the lumbar and thoracic lesions. At the cervical level, discectomies or somatotomies were performed, with or without vertebral fusion material.
The order of realization of the surgical gestures followed the cervico-thoraco-lumbar (cranio-caudal) order, even when both gestures were done at the same time. The duration of the surgery in one time was 145 minutes for the thoraco-lumbar association (thoracic osteosynthesis) and 234 minutes for the cervico-lumbar association (cervical and lumbar osteosynthesis). For those performed in two stages, the duration was on average 107 minutes per intervention. Blood loss was, for surgery in one stage, 550cc for thoraco-lumbar lesions and 1350 cc for cervico-lumbar. A blood transfusion had been performed for the latter patient. They averaged 170 cc per operating time during the two stages surgery. After a minimum follow-up of five months postoperatively, clinical improvements were noted. The results are reported in the Table 4.
The order of realization of the surgical gestures followed the cervico-thoraco-lumbar (cranio-caudal) order, even when both gestures were done at the same time. The duration of the surgery in one time was 145 minutes for the thoraco-lumbar association (thoracic osteosynthesis) and 234 minutes for the cervico-lumbar association (cervical and lumbar osteosynthesis). For those performed in two stages, the duration was on average 107 minutes per intervention. Blood loss was, for surgery in one stage, 550cc for thoraco-lumbar lesions and 1350 cc for cervico-lumbar. A blood transfusion had been performed for the latter patient. They averaged 170 cc per operating time during the two stages surgery. After a minimum follow-up of five months postoperatively, clinical improvements were noted. The results are reported in the Table 4.
4. Discussion
Although the first description of bifocal stenosis was made by Teng and Papatheodorou [1] in 1964, the term ”tandem spinal stenosis” was first used by Dagi et al [3] in 1987 to describe this particular presentation of pathology degenerative spine. Compared to all patients received in the service, for degenerative diseases of the spine, TSS represented approximately 0.96% with variations in different studies [4].
In an autopsy series, Bajwal noted a prevalence of 1% for cervico-thoracic and thoracic associations and 1.24% for thoraco-lumbar spine [5]. From a radiological study, Park found cervical and thoracic stenosis in 24% of patients with lumbar canal stenosis [6]. LaBan reported a frequency of 12/100000 admissions at all ages [7]. Molinar out of 1023 operated patients found only 9 cases of TSS or 0.87% [2]. In a multicentric study, Lui [8] found an incidence of 26.2% and higher prevalence in Chinese populations (30.7%).
The average age of our patients was 57 years, and male subjects predominated. Aiwale noted a male predominance (66.6%) and an average age of 57.8 years for men and 53.9 years for women [9]. Keiji Nagata also found a male predominance of 66.6% [10]. In a study compiling some data on the subject, Overley reported a female predominance [4]. Therefore, subject more than fifty years were more frequent as reported by LaBan [7].
The average duration of signs was 17.6 months in our series. It was 29.54±44.99 months for the cervical spine and 30.55±38 months for the lumbar spine at Aiwale [9]. The concerned clinical signs were a function of the spinal segments. In the cervico-lumbar associations, which is the most frequent anatomical site, lumbo-radiculalgia was the most reported sign among other signs (43.7%). The signs of cervical involvement were mostly found during the physical examination. It should be noted that, the presence of the thoracic spinal signs was observed in our three patients carrying damage of this segment. These different signs were found in the triad described by Dagi [3]. He recommended referring to this diagnosis of TSS in patients complaining of “numb and clumsy legs”, which are equivalents of numb and clumsy hands. The existence of pyramidal signs, in a patient consulting for lumbo-radicular signs, made us prescribe a cervical, thoracic and lumbar spinal morphological assessment, even in the absence of cervical or thoracic spinal signs [3].
Although the first description of bifocal stenosis was made by Teng and Papatheodorou [1] in 1964, the term ”tandem spinal stenosis” was first used by Dagi et al [3] in 1987 to describe this particular presentation of pathology degenerative spine. Compared to all patients received in the service, for degenerative diseases of the spine, TSS represented approximately 0.96% with variations in different studies [4].
In an autopsy series, Bajwal noted a prevalence of 1% for cervico-thoracic and thoracic associations and 1.24% for thoraco-lumbar spine [5]. From a radiological study, Park found cervical and thoracic stenosis in 24% of patients with lumbar canal stenosis [6]. LaBan reported a frequency of 12/100000 admissions at all ages [7]. Molinar out of 1023 operated patients found only 9 cases of TSS or 0.87% [2]. In a multicentric study, Lui [8] found an incidence of 26.2% and higher prevalence in Chinese populations (30.7%).
The average age of our patients was 57 years, and male subjects predominated. Aiwale noted a male predominance (66.6%) and an average age of 57.8 years for men and 53.9 years for women [9]. Keiji Nagata also found a male predominance of 66.6% [10]. In a study compiling some data on the subject, Overley reported a female predominance [4]. Therefore, subject more than fifty years were more frequent as reported by LaBan [7].
The average duration of signs was 17.6 months in our series. It was 29.54±44.99 months for the cervical spine and 30.55±38 months for the lumbar spine at Aiwale [9]. The concerned clinical signs were a function of the spinal segments. In the cervico-lumbar associations, which is the most frequent anatomical site, lumbo-radiculalgia was the most reported sign among other signs (43.7%). The signs of cervical involvement were mostly found during the physical examination. It should be noted that, the presence of the thoracic spinal signs was observed in our three patients carrying damage of this segment. These different signs were found in the triad described by Dagi [3]. He recommended referring to this diagnosis of TSS in patients complaining of “numb and clumsy legs”, which are equivalents of numb and clumsy hands. The existence of pyramidal signs, in a patient consulting for lumbo-radicular signs, made us prescribe a cervical, thoracic and lumbar spinal morphological assessment, even in the absence of cervical or thoracic spinal signs [3].
This morphological assessment, before the acquisition of the MRI, used radiological examinations namely Saccoradiculography and Myeloscanner as the first authors [1, 3]. He had allowed us to note the predominance of the cervico-lumbar associations and the absence of the triple location. The number of affected level ranged from one (especially in the cervical and lumbar) to five (only one case found at the thoracic level). For Aiwale [9], this number varied according to the spinal segment concerned. He noted a predominance of unique location in the lumbar area and more than three in the cervical one. The neurophysiological assessment that Dagi [3] and Molinar [2] proposed related to the morphological examinations in the diagnosis of these TSS was not used in our practice.
The surgery was done in one stage in two of our patients, which was the case in some patients of Bhandutia [11] and Kikuike [12]. In the other 14 cases, surgeries have been performed in two stages. Whatever the procedure (one or two stages), the surgery was done in cranio-caudal order. The fear of decompensation of high-status lesions during the installation of our patients, as reported by Chen [13] and Deem [14], was our obsession.
Probably for the same reasons, Bhandutia [11] had adopted this attitude for most of her patients. For other authors, the operative order was dictated by the importance of the symptoms. They started with the most symptomatic spinal region [3, 11, 15]. In his study, Luo [16] noted a faster decompensation of cervical signs in patients previously operated on at the lumbar level, which he did not find in patients whose procedure was reversed. He proposes this cranio-caudal order in two stages surgery.
The use of a single anesthesia for the realization of both gestures is a significant advantage, especially in old people, attributed to surgery in one time. Even the overall duration is shorter than in two-stage surgery according to Kikuike [12]. For the two patients in our study, it was 145 minutes and 234 minutes. Molinar had an average operating duration of 159 minutes with extremes of 111 to 255 minutes [2].
The participation of two surgical teams as proposed by some authors including Bhandutia [11], kikuike [12], Krishnan [17], would allow more this time. This procedure is valid in our opinion only for cervico-lumbar lesions addressed by the posterior approach. It will pose the problem of working space, in cervico-thoracic or thoraco-lumbar locations, because of the proximity of the spinal segments. This solution will also not be possible, in patients requiring anterior and posterior surgery. This one-stage surgery was a source of significant blood loss in our patients. This bleeding was estimated at 1550cc in one of our patients, and indicated a blood transfusion.
Molinar [2] reported in his study, an average bleeding of 558cc (150 to 1300cc). But, Kikuike [12], who compared the overall intraoperative bleeding of these two surgical modes, found it less important during the surgery in one stage. This constitutes another advantage of this surgery in one stage. This opinion is shared by Krishnan [17]. The postoperative evolution, satisfactory in a large number of studies, had not shown a significant difference whatever the mode or order of the surgical gestures [9, 11, 12, 15]. The determining elements of this evolution would be the duration of evolution of the signs and the speed of the realization of the surgical act according to Zulkefli [15].
The study had some strengths and limitations identified the problems related to the management of TSS in Brazzaville. These difficulties are useful bases to initiate the change of this support. The limit of the study was the reduced number of cases and its retrospective character.
5. Conclusion
The association of lumbo-radicular signs with signs of spinal cord injury should be considered for TSS, by performing a morphological assessment. Early surgery, performed in one or two stages, cranio-caudally or according to the most symptomatic level, allows a clinical improvement of these patients.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article. The participants were informed about the purpose of the research and its implementation stages; they were also assured about the confidentiality of their information. Moreover, they were allowed to leave the study whenever they wish, and if desired, the results of the research would be available to them.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' contributions
Conceptualization, methodology, and writing original draft: Leon Boukassa; Data collection: Olivier Brice Ngackosso and Sinclair Brice Kinata-Bambino; Data analysis: Hugues Brieux Ekouele Mbaki.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors would like to express their gratitude to JC Moundzika Kibamba for his contribution to this article.
Reference
Teng P, Papatheodorou C. Combined cervical and lumbar spondylosis. Archives of Neurology. 1964; 10(3):298-307. [DOI:10.1001/archneur.1964.00460150068007] [PMID]
Molinari RW, Gruhn WL, Molinari C. Tandem Spinal Stenosis (TSS): Literature review and report of patients treated with simultaneous decompression. Journal of Spine. 2014; 4(1):1000200. [DOI:10.4172/2165-7939.1000200]
Forcht Dagi T, Tarkington MA, Leech JJ. Tandem lumbar and cervical spinal stenosis: Natural history, prognostic indices, and results after surgical decompression. Journal of Neurosurgery. 1987; 66(6):842-9. [DOI:10.3171/jns.1987.66.6.0842] [PMID]
Overley SC, Kim JS, Gogel BA, Merrill RK, Hecht AC. Tandem spinal stenosis a systematic review. JBJS Reviews. 2017; 5(9):e2. [DOI:10.2106/JBJS.RVW.17.00007] [PMID]
Bajwa NS, Toy JO, Young EY, Ahn NU. Is congenital bony stenosis of the cervical spine associated with lumbar spine stenosis? An anatomical study of 1072 human cadaveric specimens. Journal of Neurosurgery: Spine. 2012; 17(1):24-9. [DO:10.3171/2012.3.SPINE111080] [PMID]
Park JY, Chin DK, Kim KS, Cho YE. Thoracic ligament ossification in patients with cervical ossification of the posterior longitudinal ligaments: Tandem ossification in the cervical and thoracic spine. Spine. 2008; 33(13):E407-E10. [DOI:10.1097/BRS.0b013e318175c276] [PMID]
LaBan MM, Green ML. Concurrent (tandem) cervical and lumbar spinal stenosis: A 10-yr review of 54 hospitalized patients. American Journal of Physical Medicine & Rehabilitation. 2004; 83(3):187-90. [DOI:10.1097/01.PHM.0000113405.48879.45] [PMID]
Liu G, Tan B, Riew D, Wong HK. Tandem spinal stenosis: A 926 multiracial Asian patients’ prevalence and risk factors analysis. Orthopaedic Proceedings. 2018; 96-B(Suppl 11):296. [DOI:10.1302/1358-992X.96BSUPP_11.CORS2013-296]
Aiwale AB, Patel PR, Paspala SAB, Ramakrishna Murthy TV. Simultaneous cervical and lumbar spine surgery: Retrospective analysis of 45 cases. Indian Journal of Neurosurgery. 2019; 08(01):047-052. [DOI:10.1055/s-0039-1677962]
Nagata K, Yoshimura N, Hashizume H, Ishimoto Y, Muraki Sh, Yamada H, et al. The prevalence of tandem spinal stenosis and its characteristics in a population-based MRI study: The Wakayama Spine Study. European Spine Journal. 2017; 26:2529-35. [DOI:10.1007/s00586-017-5072-0] [PMID]
Bhandutia A, Brown L, Nash A, Bussey I, Shasti M, Koh E, et al. Delayed diagnosis of tandem spinal stenosis: A retrospective institutional review. International Journal of Spine Surgery. 2019; 13(3):283-8. [DOI:10.14444/6038] [PMID] [PMCID]
Kikuike K, Miyamoto K, Hosoe H, Shimizu K. One-staged combined cervical and lumbar decompression for patients with tandem spinal stenosis on cervical and lumbar spine: Analyses of clinical outcomes with minimum 3 years follow-up. Journal of Spinal Disorders & Techniques. 2009; 22(8):593-601. [DOI:10.1097/BSD.0b013e3181929cbd] [PMID]
Chen SH, Hui YL, Yu CM, Niu CC, Lui PW. Paraplegia by acute cervical disc protrusion after lumbar spine surgery. Chang Gung Medical Journal. 2005; 28(4):254-7.
Deem S, Shapiro HM, Marshall LF. Quadriplegia in a patient with cervical spondylosis after thoracolumbar surgery in the prone position. Anesthesiology. 1991; 75(3):527-8. [DOI:10.1097/00000542-199109000-00022] [PMID]
Zulkefli A, Ramanathan R. Tandem spinal stenosis. Malaysian Orthopaedic Journal. 2010; 4(1):46-9. [DOI:10.5704/MOJ.1003.010]
Luo CA, KaliyaPerumal AK, Lu ML, Chen LH, Chen WJ, Niu CC. Staged surgery for tandem cervical and lumbar spinal stenosis: Which should be treated first? European Spine Journal volume. 2019; 28:61-8. [DOI:10.1007/s00586-018-5795-6] [PMID]
Krishnan A, Dave BR, Kambar AK, Ram H. Coexisting lumbar and cervical stenosis (tandem spinal stenosis): An infrequent presentation. Retrospective analysis of single-stage surgery (53 cases). European Spine Journal. 2014; 23(1):64-73. [DOI:10.1007/s00586-013-2868-4] [PMID] [PMCID]
The surgery was done in one stage in two of our patients, which was the case in some patients of Bhandutia [11] and Kikuike [12]. In the other 14 cases, surgeries have been performed in two stages. Whatever the procedure (one or two stages), the surgery was done in cranio-caudal order. The fear of decompensation of high-status lesions during the installation of our patients, as reported by Chen [13] and Deem [14], was our obsession.
Probably for the same reasons, Bhandutia [11] had adopted this attitude for most of her patients. For other authors, the operative order was dictated by the importance of the symptoms. They started with the most symptomatic spinal region [3, 11, 15]. In his study, Luo [16] noted a faster decompensation of cervical signs in patients previously operated on at the lumbar level, which he did not find in patients whose procedure was reversed. He proposes this cranio-caudal order in two stages surgery.
The use of a single anesthesia for the realization of both gestures is a significant advantage, especially in old people, attributed to surgery in one time. Even the overall duration is shorter than in two-stage surgery according to Kikuike [12]. For the two patients in our study, it was 145 minutes and 234 minutes. Molinar had an average operating duration of 159 minutes with extremes of 111 to 255 minutes [2].
The participation of two surgical teams as proposed by some authors including Bhandutia [11], kikuike [12], Krishnan [17], would allow more this time. This procedure is valid in our opinion only for cervico-lumbar lesions addressed by the posterior approach. It will pose the problem of working space, in cervico-thoracic or thoraco-lumbar locations, because of the proximity of the spinal segments. This solution will also not be possible, in patients requiring anterior and posterior surgery. This one-stage surgery was a source of significant blood loss in our patients. This bleeding was estimated at 1550cc in one of our patients, and indicated a blood transfusion.
Molinar [2] reported in his study, an average bleeding of 558cc (150 to 1300cc). But, Kikuike [12], who compared the overall intraoperative bleeding of these two surgical modes, found it less important during the surgery in one stage. This constitutes another advantage of this surgery in one stage. This opinion is shared by Krishnan [17]. The postoperative evolution, satisfactory in a large number of studies, had not shown a significant difference whatever the mode or order of the surgical gestures [9, 11, 12, 15]. The determining elements of this evolution would be the duration of evolution of the signs and the speed of the realization of the surgical act according to Zulkefli [15].
The study had some strengths and limitations identified the problems related to the management of TSS in Brazzaville. These difficulties are useful bases to initiate the change of this support. The limit of the study was the reduced number of cases and its retrospective character.
5. Conclusion
The association of lumbo-radicular signs with signs of spinal cord injury should be considered for TSS, by performing a morphological assessment. Early surgery, performed in one or two stages, cranio-caudally or according to the most symptomatic level, allows a clinical improvement of these patients.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article. The participants were informed about the purpose of the research and its implementation stages; they were also assured about the confidentiality of their information. Moreover, they were allowed to leave the study whenever they wish, and if desired, the results of the research would be available to them.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' contributions
Conceptualization, methodology, and writing original draft: Leon Boukassa; Data collection: Olivier Brice Ngackosso and Sinclair Brice Kinata-Bambino; Data analysis: Hugues Brieux Ekouele Mbaki.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors would like to express their gratitude to JC Moundzika Kibamba for his contribution to this article.
Reference
Teng P, Papatheodorou C. Combined cervical and lumbar spondylosis. Archives of Neurology. 1964; 10(3):298-307. [DOI:10.1001/archneur.1964.00460150068007] [PMID]
Molinari RW, Gruhn WL, Molinari C. Tandem Spinal Stenosis (TSS): Literature review and report of patients treated with simultaneous decompression. Journal of Spine. 2014; 4(1):1000200. [DOI:10.4172/2165-7939.1000200]
Forcht Dagi T, Tarkington MA, Leech JJ. Tandem lumbar and cervical spinal stenosis: Natural history, prognostic indices, and results after surgical decompression. Journal of Neurosurgery. 1987; 66(6):842-9. [DOI:10.3171/jns.1987.66.6.0842] [PMID]
Overley SC, Kim JS, Gogel BA, Merrill RK, Hecht AC. Tandem spinal stenosis a systematic review. JBJS Reviews. 2017; 5(9):e2. [DOI:10.2106/JBJS.RVW.17.00007] [PMID]
Bajwa NS, Toy JO, Young EY, Ahn NU. Is congenital bony stenosis of the cervical spine associated with lumbar spine stenosis? An anatomical study of 1072 human cadaveric specimens. Journal of Neurosurgery: Spine. 2012; 17(1):24-9. [DO:10.3171/2012.3.SPINE111080] [PMID]
Park JY, Chin DK, Kim KS, Cho YE. Thoracic ligament ossification in patients with cervical ossification of the posterior longitudinal ligaments: Tandem ossification in the cervical and thoracic spine. Spine. 2008; 33(13):E407-E10. [DOI:10.1097/BRS.0b013e318175c276] [PMID]
LaBan MM, Green ML. Concurrent (tandem) cervical and lumbar spinal stenosis: A 10-yr review of 54 hospitalized patients. American Journal of Physical Medicine & Rehabilitation. 2004; 83(3):187-90. [DOI:10.1097/01.PHM.0000113405.48879.45] [PMID]
Liu G, Tan B, Riew D, Wong HK. Tandem spinal stenosis: A 926 multiracial Asian patients’ prevalence and risk factors analysis. Orthopaedic Proceedings. 2018; 96-B(Suppl 11):296. [DOI:10.1302/1358-992X.96BSUPP_11.CORS2013-296]
Aiwale AB, Patel PR, Paspala SAB, Ramakrishna Murthy TV. Simultaneous cervical and lumbar spine surgery: Retrospective analysis of 45 cases. Indian Journal of Neurosurgery. 2019; 08(01):047-052. [DOI:10.1055/s-0039-1677962]
Nagata K, Yoshimura N, Hashizume H, Ishimoto Y, Muraki Sh, Yamada H, et al. The prevalence of tandem spinal stenosis and its characteristics in a population-based MRI study: The Wakayama Spine Study. European Spine Journal. 2017; 26:2529-35. [DOI:10.1007/s00586-017-5072-0] [PMID]
Bhandutia A, Brown L, Nash A, Bussey I, Shasti M, Koh E, et al. Delayed diagnosis of tandem spinal stenosis: A retrospective institutional review. International Journal of Spine Surgery. 2019; 13(3):283-8. [DOI:10.14444/6038] [PMID] [PMCID]
Kikuike K, Miyamoto K, Hosoe H, Shimizu K. One-staged combined cervical and lumbar decompression for patients with tandem spinal stenosis on cervical and lumbar spine: Analyses of clinical outcomes with minimum 3 years follow-up. Journal of Spinal Disorders & Techniques. 2009; 22(8):593-601. [DOI:10.1097/BSD.0b013e3181929cbd] [PMID]
Chen SH, Hui YL, Yu CM, Niu CC, Lui PW. Paraplegia by acute cervical disc protrusion after lumbar spine surgery. Chang Gung Medical Journal. 2005; 28(4):254-7.
Deem S, Shapiro HM, Marshall LF. Quadriplegia in a patient with cervical spondylosis after thoracolumbar surgery in the prone position. Anesthesiology. 1991; 75(3):527-8. [DOI:10.1097/00000542-199109000-00022] [PMID]
Zulkefli A, Ramanathan R. Tandem spinal stenosis. Malaysian Orthopaedic Journal. 2010; 4(1):46-9. [DOI:10.5704/MOJ.1003.010]
Luo CA, KaliyaPerumal AK, Lu ML, Chen LH, Chen WJ, Niu CC. Staged surgery for tandem cervical and lumbar spinal stenosis: Which should be treated first? European Spine Journal volume. 2019; 28:61-8. [DOI:10.1007/s00586-018-5795-6] [PMID]
Krishnan A, Dave BR, Kambar AK, Ram H. Coexisting lumbar and cervical stenosis (tandem spinal stenosis): An infrequent presentation. Retrospective analysis of single-stage surgery (53 cases). European Spine Journal. 2014; 23(1):64-73. [DOI:10.1007/s00586-013-2868-4] [PMID] [PMCID]
Type of Study: Clinical Trial |
Subject:
Spine
Send email to the article author
| Rights and Permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |