Thu, Jul 3, 2025
Volume 6, Issue 1 (Winter 2020)
Iran J Neurosurg 2020, 6(1): 41-48 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Garg D, Jain G, Sinha V. A Case Report of Primary Brain Hydatid Cyst in a Child. Iran J Neurosurg 2020; 6 (1) :41-48
URL: http://irjns.org/article-1-198-en.html
URL: http://irjns.org/article-1-198-en.html
1- MCH Neurosurgery, Senior Resident, SMS Medical College, Jaipur, India
2- DNB Neurosurgery, Assistant Professor, SMS Medical College, Jaipur, India ,drgauravjain9@gmail.com
3- MCH Neurosurgery, Senior Professor, SMS Medical College, Jaipur, India
2- DNB Neurosurgery, Assistant Professor, SMS Medical College, Jaipur, India ,
3- MCH Neurosurgery, Senior Professor, SMS Medical College, Jaipur, India
Full Text [PDF 917 kb]
(1819 Downloads)
| Abstract (HTML) (4128 Views)
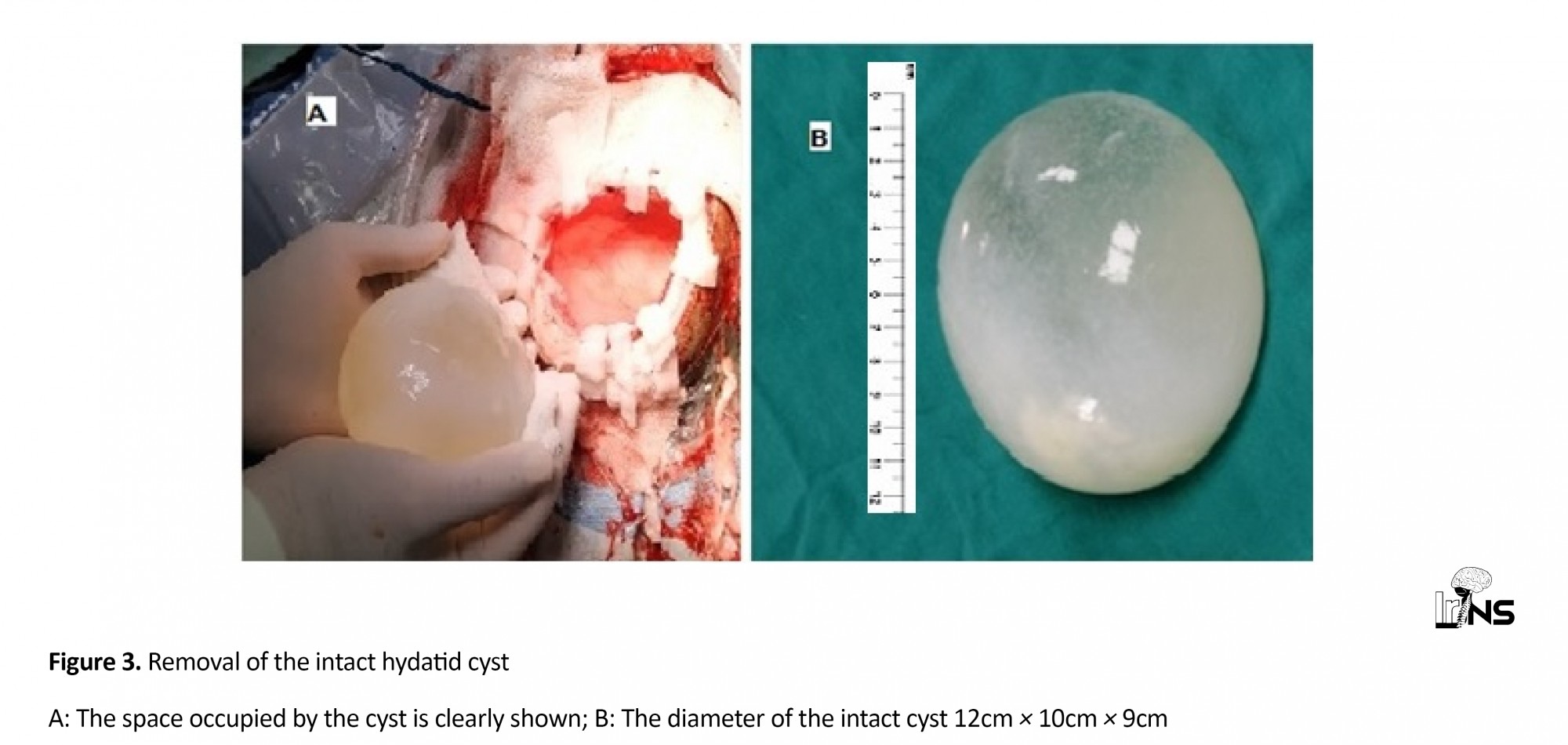
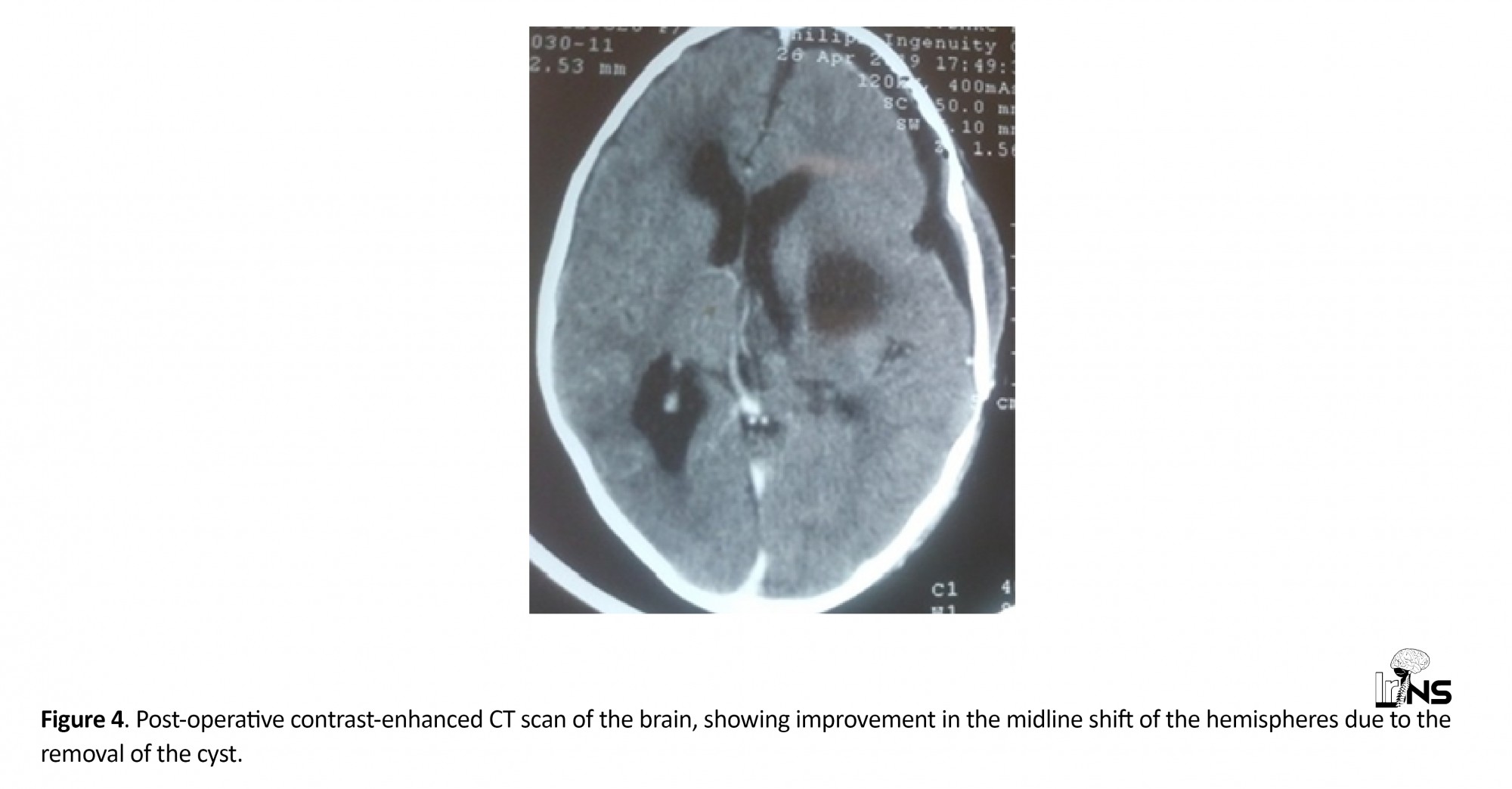
Head CT scan showed a very large intraparenchymal hypodense lesion involving the left fronto-parietal region, with no contrast enhancement and no diffusion restriction on MRI. There was also no associated perilesional edema on brain MRI (Figure 1A-D). After a trial of empirical albendazole, the patient underwent a large craniotomy to remove the cyst. The cyst was removed totally intact via the Dowling's technique (Figures 2, 3A and 3B) [3, 4]. Post-operative contrast-enhanced CT revealed the complete removal of the cyst (Figure 4). After an uneventful recovery, the patient was given a treatment regime of 10 mg/kg/day albendazole for six months and follow-up showed no recurrence during clinical examinations. Chest X-ray and ultrasonography of the abdomen was done at every follow-up session and the brain CT was done at month three post-operation. Complete improvement in the speech was achieved in the first-month post-operation, and complete improvement in right facial nerve palsy and right side limb weakness was achieved in the month three post-operation.
3. Discussion
3.1. Pathogenesis
Hydatid cyst is an infectious disease whichbegins with the entrance of the larval stage of dog tapeworm (Echinococcus granulosus and Echinococcus multilocularis) in the human body passed on via exposure to a definitive host (generally a dog) or by eating contaminated water or vegetables. Hydatid cyst has two layers, an outer pericyte layer, which is composed of a fibrocollagenous lamellated chitinous layer, and an inner germinal layer, accompanied by brood capsule and hooklets embedded in it. Generally, the cyst remains asymptomatic until an intra-organ mass affects it and it gets ruptured [3].
Brain involvement in hydatid cyst disease may occur as primary or secondary. The former happens when the larva escapes the liver and lung filtration barriers and directly enters into the brain, while the latter develops secondary to a hydatid cyst rupture in another organ with the resultant brain involvement via blood stream.
Primary cysts are most of the times solitary and fertile, but secondary cysts are generally multiple and infertile [4, 5]. The proposed mechanisms for the development of primary brain hydatid cyst are defective immune system within the brain parenchyma, the presence of cardiac anomalies like patent ductus arteriosus, and patent foramen ovale.
The higher affinity of the certain genotype of E. granulosus for the brain and variations in class II HLA in normal population leads to a different rate of susceptibility to hydatidosis [1, 5].
The majority of the cerebral hydatid cysts (75%) occur in the pediatric age group, being two to three times more common than in adults [1]. In our study, the patient was a female child, but in the literature, male predominance was found (i.e. 50%-70%) [5]. The most common site in the brain is the parietal lobe [5]. Other uncommon brain regions are the calvarium, eyeball, cavernous sinus, cerebellum, pons, ventricles, and extradural region [6]. Most reported cases had solitary, intraparenchymal cysts in the supratentorial region and in the vicinity of the middle cerebral artery [7].
Particularly in pediatric age, the elasticity of calvarium and high compressibility of brain tissue leads to high growth rate and development of the large size of brain hydatid cysts [8]. The rate of growth in the brain is usually faster than in any other organ and it is said to be around 4.5 cm/6 months [1]. Tuzun et al. stated that other organs’ involvement with brain hydatid reaches up to 80-90% in post-mortem examinations, whereas in clinical practice, concomitant extracranial cysts were rarely demonstrated. The hydatid cysts in other organs are too small to be diagnosed by clinical and radiological evaluations [1].
3.2. Clinical presentation
Clinical features vary accordingtothe size of the hydatid cyst and its location. Patients mostly present with headache and vomiting as a result of increased Intracranial Pressure (ICP). Other manifestations are seizures, hemiparesis, visual disturbances, speech difficulties, cranial nerve deficit, and ataxic gaits. Papilledema is mostly present at the first hospital visit in children [1]. In our study, the child did not have headache or vomiting and presented with slurring of speech, right UMN type facial palsy, and right-side hemiparesis.
3.3. Differential diagnosis
Differential diagnoses of hydatid cyst are the other brain cystic masses in pediatric patients like a pyogenic or fungal abscess, cystic astrocytoma, cystic granuloma, arachnoid cyst, and porencephalic cyst. Pilocytic astrocytoma enhances in CT and MRI and has a characteristic feature which is known as a contrast-enhancing nodule (moral nodule). Although arachnoid cysts occupy an extra-axial location like hydatid cysts, they are not as round as hydatid cysts and are not surrounded by the brain tissue.
Abscesses have a thick wall, which brilliantly enhances with contrast, and the edema surrounding it. In neurocysticercosis, multiple cysts are seen in different stages, and in fact, they have a pattern called "hole-with dot", as the larval scolex could existas a mural nodule [9].
3.3.1. Serology
The cutaneous test described by Casoni, the complement fixation reaction described by Ghedini and Weinberg, indirect hemagglutination, ELISA, and eosinophilia were classically used to diagnose hydatid cyst. Nevertheless, as a minimal response would be elicited within the brain in cerebral hydatidosis, false-negative results may occur frequently [2]. Hence, serologic studies are of little clinical importance in brain hydatid cyst [4, 10].
3.3.2. Radiology
Brain CT and MRI are not the only keys to radiological diagnosis, but they are also beneficial for planning the surgery. Brain CT displays hydatid cysts as intra-axial, homogenous cystic lesions with well-defined borders. The cyst fluid is isodense with the Cerebrospinal Fluid (CSF), and the cyst itself is usually round. Non-contrast CT scans display hypodense, well-circumscribed, and circular cysts compared to the brain tissue. The perilesional edema and enhancement of contrast seen with abscesses or cystic tumors are unusual for brain hydatid cysts [11]. MRI displays brain hydatid cysts as hypo-intense on T1 weighted image, and it appears as a hyper-intense region on T2 weighted image with a hypo-intense disc surrounding the cyst. Excellent peripheral enhancement accompanying perilesional edema may be present in active inflammation, although calcifications are only seen in 1% of the cases. Though, alveolar hydatid appear as a contrast-enhancing solid cystic lesion with perilesional edema, and calcification [11]. Measuring reliable markers such as alanine, succinate, acetate and lactate on Magnetic Resonance Spectroscopy (MRS) before and after treatment is an excellent indicator of efficient chemotherapy [2].
3.4. Treatment
3.4.1. Medical management
Albendazole is currently the drug of choice; it inhibits the uptake of glucose by both the larva and the adult worm. This results in depletion of their glycogen storage which subsequently leads to diminished Adenosine Triphosphate (ATP) production, causing death of the larva and adult worm [5]. Albendazole is effective as it sterilizes the cyst, decreases the anaphylaxis risk, and reduces the rate of recurrence [10]. In some case reports, effective disappearance of multiple brain hydatid cysts with daily doses of albendazole, given three times of 10 mg/kg for a period of four months has been reported [12]. Some studies have also reported the effective disappearance of around 48% of the cysts and prominent reduction in the size of 28% of the cysts following albendazole treatment [2].
It should be noted that mebendazole and albendazole are teratogenic drugs and should not be used for pregnant patients [1]. These drugs are recommended at least for six months [7], and monitoring should be done with clinical and radiological evaluation. In the case of Echinococcus. multilocularis infection, these drugs should be given to the patients for up to two years. In patients with inoperable lesions, it might be necessary to use the drugs as long as possible, even to the end of life [6]. That way, albendazole is given at the dose of 10-15 mg/kg/day in two divided doses. In case of non-tolerable side effects to albendazole, mebendazole is given 40-50 mg/kg/day [13].
3.4.2. Surgical management
Surgery is the treatment of choice for hydatid cyst, and aims to complete excision without rupture, to prevent recurrence and immunological reaction. Many techniques for hydatid cyst excision have been investigated, all of which have reached a consensus on the necessity of an atraumatic removal of the cyst to avoid rupture.
The Dowling's technique has been used as the preferred operative technique for CNS hydatid cysts. During which the delivery of the cyst is done by declining the head of the operating table by 30 degrees and hydro-dissection and Valsalva. This is feasible due fragile adhesions around the cyst wall [14]. Although lowering the ICP by anesthetists is a critical step to provide better access to the cyst, in some cases a small increments in ICP is required to help the cyst being pushed out.
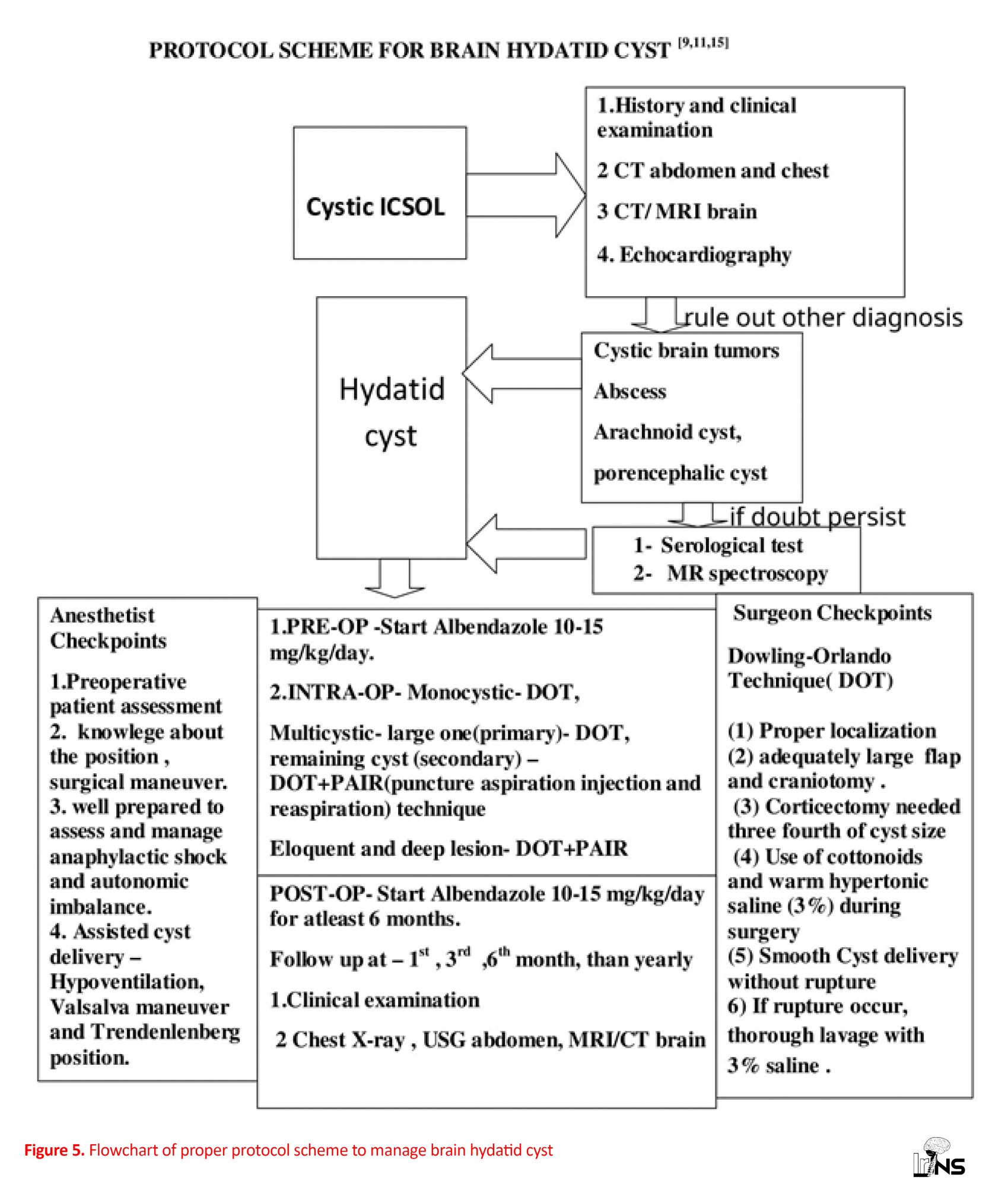
In such cases, hypoventilation is done to increase the PaCO2 and the Valsalva maneuver may be used in Trendelenburg position [15]. High index of suspicion is required to diagnose an anaphylactic reaction and to manage it byearly aggressive surgical treatment and delivering 100% oxygen with epinephrine infusion and massive fluid resuscitation. To prevent and treat the refractory hypotension, prophylactic hydrocortisone supplementation is also recommended [15]. The proper protocol should be followed as represented in the schematic flowchart (Figure 5).
3.4.3. Complications
An intra-operative rupture of hydatid cysts can lead to fatal anaphylactic reaction and a high chance of recurrence [12]. The reported recurrence rate in the brain due to cyst rupture at surgery is reported 40.7% [1]. Mainly reported post-operative complications are hemorrhage, seizures, subdural effusion, porencephalic cyst, hydrocephalus, pneumocephalus, and focal neurological deficits, which sometime may need further intervention [7]. The space left after the excision of large hydatid cysts may lead to fatal complications, such as subdural hematomas, hyperpyrexia, cerebral edema, cortical collapse, or cardiorespiratory failure, in the early post-operative days. In late post-operative days the rate of complication such as subdural effusion and the porencephalic cyst. Cortical collapse associated with mortality is around 0.07 [16]. Majority of cases with neurological deficits improved completely as Hilmani et al. described 90% recovery in the neurological deficits in their case series [5].
4. Conclusion
In endemic countries (even in non-endemic countries due to migration), while considering differentials for cystic masses of the brain, the hydatid cyst disease has an important place. Its rupture can be detrimental for the patient, so proper protocol should be followed for complete excision to prevent anaphylactic reaction and dissemination.
Ethical Considerations
Compliance with ethical guidelines
This research was approved by the Ethics Committee of SMS Hospital, Jaipur, India.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
All authors have contributed equally to the manuscript.
Conflict of interest
The authors declare no conflict of interest.
References
Khalifa RMA, Mahmoud AE, Othman RM. Spotlight on the hydatid cyst and whether its location is accidental or target. Parasitol United Journal. 2015; 8(1):4-13. [DOI:10.4103/1687-7942.163403]
Nemati A, Kamgarpour A, Rashid M, Nazari SS. Giant cerebral hydatid cyst in a child: A case report and review of the literature. British Journal of Medical Practitioners (BJMP). 2010; 3(3):a338.
Luo K, Luo DH, Zhang TR, Wen H. Primary intracranial and spinal hydatidosis: A retrospective study of 21 cases. Pathog Glob Health. 2013; 107(2):47-51. [DOI:10.1179/2047773213Y.0000000072] [PMID] [PMCID]
Tuzun Y, Kadioglu HH, Izci Y, Suma S, Keles M, Aydin IH. The clinical, radiological, and surgical aspects of cerebral hydatid cysts in children. Pediatric Neurosurgery. 2004; 40(4):155-60. [DOI:10.1159/000081932] [PMID]
Hilmani S. Brain hydatid cyst. In: Echinococcosis. Alfonso J. Rodriguez-Morales. IntechOpen; 2015. [DOI:10.5772/60820]
Gupta S, Desai K, Goel A. Intracranial hydatid cyst: A report of five cases and review of the literature. Neurol India. 1999; 47:214
Ersahin Y, Mutluer S, Guzelbag E. Intracranial hydatid cysts in children. Neurosurgery. 1993; 33(2):219-24. [DOI:10.1097/00006123-199308000-00006] [PMID]
Debourgogne A, Goehringer F, Umhang G, Gauchotte G, Hénard S, Boué F, et al. Primary cerebral alveolar echinococcosis: Mycology to the rescue. Journal of Clinical Microbiology. 2014; 52(2):692-94. [DOI:10.1128/JCM.02843-13] [PMID] [PMCID]
Alok R, Mahmoud J. Successful surgical treatment of a brain stem hydatid cyst in a child. Case Reports in Surgery. 2020; 2020:1-3. [DOI:10.1155/2020/5645812] [PMID] [PMCID]
Imperato A, Consales A, Ravegnani M, Castagnola E, Bandettini R, Rossi A. Primaryhydatid cyst of the brain in a child. Polish Journal of Radiology. 2016; 81:578-82. [DOI:10.12659/PJR.898619] [PMID] [PMCID]
Altibi AM, Qarajeh RA, Belsuzarri TA, Maani W, Kanaan TM. Primary cerebral echinococcosis in a child: A case report - Surgical technique, technical pitfalls, and video atlas. Surgical Neurology International. 2016; 7:S893-8. [DOI:10.4103/2152-7806.194512] [PMID] [PMCID]
Senapati SB, Parida DK, Pattajoshi AS, Gouda AK, Patnaik A. Primary hydatid cyst of the brain: Two cases report. Asian Journal of Neurosurgery. 2015; 10(2):175-6. [DOI:10.4103/1793-5482.152109] [PMID] [PMCID]
Lotfinia I. Central nervous system hydatid disease. [Internet]. 2017 [Cited 2017 Feb 23 ]; Available from: https://smjournals.com/ebooks/monographs/chapters/MONO-17-02.pdf
Arora SK, Aggarwal A, Datta V. Giant primary cerebral hydatid cyst: A rare cause of childhood seizure. Journal of Pediatric Neurosciences. 2014; 9(1):73-5. [DOI:10.4103/1817-1745.131495] [PMID] [PMCID]
Nashibi M, Tafrishinejad A, Hussain Khan Z. Deep seated cerebral hydatid cyst and it’s anesthetic considerations: A case report. Archives of Neuroscience. 2020; 7(1):e100044. [DOI:10.5812/ans.100044]
Cavusoglu H, tuncer C ozdilmac A, Aydin Y. Multiple intracranial hydatid cysts in a boy. Turkish Neurosurgery. 2009; 19(2):203-7. [PMID]
Full Text: (2918 Views)
1. Introduction
n tropical countries, hydatid disease contributes to a major health burden among zoonotic diseases. Hydatid disease is endemic in Libya, Tunisia, Algeria, Iran, Iraq, Turkey, Morocco, Egypt, and India [1]. But today, some cases are seen in non-endemic regions as a result of migration. The most involved organ by the hydatid cyst is the liver (77%). The less frequently involved organs are the lungs (43%), kidneys (2%), heart (2%), brain (2%), eye (1%), spinal cord (1%), spleen, spermatic cord, and soft tissues [2]. The highest prevalence rate is reported in the Mediterranean region, which is around 8% [2]. Hydatid cyst can have spontaneous, traumatic, or even iatrogenic rupture. Thus, misdiagnosis can lead to anaphylactic reactions and dissemination. To avoid this, the brain surgeon should keep a high level of suspicion in mind for brain hydatidosis, when a patient presents with an intracerebral cystic lesion in endemic countries.
2. Case Presentation
An eight-year-old girl presented progressive right-sided hemiparesis, left deviation of the angle of the mouth, and slurred speech for two and a half months as main complaints. She had no history of headache, seizure episode, or any pet exposure. On examination, there was apparent Left central facial palsy, and power in the right upper and lower limbs were MRC grade 3/5 and 4/5, respectively. A Grade II papilledema (Frisen scale) was detected bilaterally. All other investigations including routine blood test, chest X-rays, chest and abdomen Computed Tomography (CT), and echocardiography were within normal range.
n tropical countries, hydatid disease contributes to a major health burden among zoonotic diseases. Hydatid disease is endemic in Libya, Tunisia, Algeria, Iran, Iraq, Turkey, Morocco, Egypt, and India [1]. But today, some cases are seen in non-endemic regions as a result of migration. The most involved organ by the hydatid cyst is the liver (77%). The less frequently involved organs are the lungs (43%), kidneys (2%), heart (2%), brain (2%), eye (1%), spinal cord (1%), spleen, spermatic cord, and soft tissues [2]. The highest prevalence rate is reported in the Mediterranean region, which is around 8% [2]. Hydatid cyst can have spontaneous, traumatic, or even iatrogenic rupture. Thus, misdiagnosis can lead to anaphylactic reactions and dissemination. To avoid this, the brain surgeon should keep a high level of suspicion in mind for brain hydatidosis, when a patient presents with an intracerebral cystic lesion in endemic countries.
2. Case Presentation
An eight-year-old girl presented progressive right-sided hemiparesis, left deviation of the angle of the mouth, and slurred speech for two and a half months as main complaints. She had no history of headache, seizure episode, or any pet exposure. On examination, there was apparent Left central facial palsy, and power in the right upper and lower limbs were MRC grade 3/5 and 4/5, respectively. A Grade II papilledema (Frisen scale) was detected bilaterally. All other investigations including routine blood test, chest X-rays, chest and abdomen Computed Tomography (CT), and echocardiography were within normal range.
Head CT scan showed a very large intraparenchymal hypodense lesion involving the left fronto-parietal region, with no contrast enhancement and no diffusion restriction on MRI. There was also no associated perilesional edema on brain MRI (Figure 1A-D). After a trial of empirical albendazole, the patient underwent a large craniotomy to remove the cyst. The cyst was removed totally intact via the Dowling's technique (Figures 2, 3A and 3B) [3, 4]. Post-operative contrast-enhanced CT revealed the complete removal of the cyst (Figure 4). After an uneventful recovery, the patient was given a treatment regime of 10 mg/kg/day albendazole for six months and follow-up showed no recurrence during clinical examinations. Chest X-ray and ultrasonography of the abdomen was done at every follow-up session and the brain CT was done at month three post-operation. Complete improvement in the speech was achieved in the first-month post-operation, and complete improvement in right facial nerve palsy and right side limb weakness was achieved in the month three post-operation.
3. Discussion
3.1. Pathogenesis
Hydatid cyst is an infectious disease whichbegins with the entrance of the larval stage of dog tapeworm (Echinococcus granulosus and Echinococcus multilocularis) in the human body passed on via exposure to a definitive host (generally a dog) or by eating contaminated water or vegetables. Hydatid cyst has two layers, an outer pericyte layer, which is composed of a fibrocollagenous lamellated chitinous layer, and an inner germinal layer, accompanied by brood capsule and hooklets embedded in it. Generally, the cyst remains asymptomatic until an intra-organ mass affects it and it gets ruptured [3].
Brain involvement in hydatid cyst disease may occur as primary or secondary. The former happens when the larva escapes the liver and lung filtration barriers and directly enters into the brain, while the latter develops secondary to a hydatid cyst rupture in another organ with the resultant brain involvement via blood stream.
Primary cysts are most of the times solitary and fertile, but secondary cysts are generally multiple and infertile [4, 5]. The proposed mechanisms for the development of primary brain hydatid cyst are defective immune system within the brain parenchyma, the presence of cardiac anomalies like patent ductus arteriosus, and patent foramen ovale.
The higher affinity of the certain genotype of E. granulosus for the brain and variations in class II HLA in normal population leads to a different rate of susceptibility to hydatidosis [1, 5].
The majority of the cerebral hydatid cysts (75%) occur in the pediatric age group, being two to three times more common than in adults [1]. In our study, the patient was a female child, but in the literature, male predominance was found (i.e. 50%-70%) [5]. The most common site in the brain is the parietal lobe [5]. Other uncommon brain regions are the calvarium, eyeball, cavernous sinus, cerebellum, pons, ventricles, and extradural region [6]. Most reported cases had solitary, intraparenchymal cysts in the supratentorial region and in the vicinity of the middle cerebral artery [7].
Particularly in pediatric age, the elasticity of calvarium and high compressibility of brain tissue leads to high growth rate and development of the large size of brain hydatid cysts [8]. The rate of growth in the brain is usually faster than in any other organ and it is said to be around 4.5 cm/6 months [1]. Tuzun et al. stated that other organs’ involvement with brain hydatid reaches up to 80-90% in post-mortem examinations, whereas in clinical practice, concomitant extracranial cysts were rarely demonstrated. The hydatid cysts in other organs are too small to be diagnosed by clinical and radiological evaluations [1].
3.2. Clinical presentation
Clinical features vary accordingtothe size of the hydatid cyst and its location. Patients mostly present with headache and vomiting as a result of increased Intracranial Pressure (ICP). Other manifestations are seizures, hemiparesis, visual disturbances, speech difficulties, cranial nerve deficit, and ataxic gaits. Papilledema is mostly present at the first hospital visit in children [1]. In our study, the child did not have headache or vomiting and presented with slurring of speech, right UMN type facial palsy, and right-side hemiparesis.
3.3. Differential diagnosis
Differential diagnoses of hydatid cyst are the other brain cystic masses in pediatric patients like a pyogenic or fungal abscess, cystic astrocytoma, cystic granuloma, arachnoid cyst, and porencephalic cyst. Pilocytic astrocytoma enhances in CT and MRI and has a characteristic feature which is known as a contrast-enhancing nodule (moral nodule). Although arachnoid cysts occupy an extra-axial location like hydatid cysts, they are not as round as hydatid cysts and are not surrounded by the brain tissue.
Abscesses have a thick wall, which brilliantly enhances with contrast, and the edema surrounding it. In neurocysticercosis, multiple cysts are seen in different stages, and in fact, they have a pattern called "hole-with dot", as the larval scolex could existas a mural nodule [9].
3.3.1. Serology
The cutaneous test described by Casoni, the complement fixation reaction described by Ghedini and Weinberg, indirect hemagglutination, ELISA, and eosinophilia were classically used to diagnose hydatid cyst. Nevertheless, as a minimal response would be elicited within the brain in cerebral hydatidosis, false-negative results may occur frequently [2]. Hence, serologic studies are of little clinical importance in brain hydatid cyst [4, 10].
3.3.2. Radiology
Brain CT and MRI are not the only keys to radiological diagnosis, but they are also beneficial for planning the surgery. Brain CT displays hydatid cysts as intra-axial, homogenous cystic lesions with well-defined borders. The cyst fluid is isodense with the Cerebrospinal Fluid (CSF), and the cyst itself is usually round. Non-contrast CT scans display hypodense, well-circumscribed, and circular cysts compared to the brain tissue. The perilesional edema and enhancement of contrast seen with abscesses or cystic tumors are unusual for brain hydatid cysts [11]. MRI displays brain hydatid cysts as hypo-intense on T1 weighted image, and it appears as a hyper-intense region on T2 weighted image with a hypo-intense disc surrounding the cyst. Excellent peripheral enhancement accompanying perilesional edema may be present in active inflammation, although calcifications are only seen in 1% of the cases. Though, alveolar hydatid appear as a contrast-enhancing solid cystic lesion with perilesional edema, and calcification [11]. Measuring reliable markers such as alanine, succinate, acetate and lactate on Magnetic Resonance Spectroscopy (MRS) before and after treatment is an excellent indicator of efficient chemotherapy [2].
3.4. Treatment
3.4.1. Medical management
Albendazole is currently the drug of choice; it inhibits the uptake of glucose by both the larva and the adult worm. This results in depletion of their glycogen storage which subsequently leads to diminished Adenosine Triphosphate (ATP) production, causing death of the larva and adult worm [5]. Albendazole is effective as it sterilizes the cyst, decreases the anaphylaxis risk, and reduces the rate of recurrence [10]. In some case reports, effective disappearance of multiple brain hydatid cysts with daily doses of albendazole, given three times of 10 mg/kg for a period of four months has been reported [12]. Some studies have also reported the effective disappearance of around 48% of the cysts and prominent reduction in the size of 28% of the cysts following albendazole treatment [2].
It should be noted that mebendazole and albendazole are teratogenic drugs and should not be used for pregnant patients [1]. These drugs are recommended at least for six months [7], and monitoring should be done with clinical and radiological evaluation. In the case of Echinococcus. multilocularis infection, these drugs should be given to the patients for up to two years. In patients with inoperable lesions, it might be necessary to use the drugs as long as possible, even to the end of life [6]. That way, albendazole is given at the dose of 10-15 mg/kg/day in two divided doses. In case of non-tolerable side effects to albendazole, mebendazole is given 40-50 mg/kg/day [13].
3.4.2. Surgical management
Surgery is the treatment of choice for hydatid cyst, and aims to complete excision without rupture, to prevent recurrence and immunological reaction. Many techniques for hydatid cyst excision have been investigated, all of which have reached a consensus on the necessity of an atraumatic removal of the cyst to avoid rupture.
The Dowling's technique has been used as the preferred operative technique for CNS hydatid cysts. During which the delivery of the cyst is done by declining the head of the operating table by 30 degrees and hydro-dissection and Valsalva. This is feasible due fragile adhesions around the cyst wall [14]. Although lowering the ICP by anesthetists is a critical step to provide better access to the cyst, in some cases a small increments in ICP is required to help the cyst being pushed out.
In such cases, hypoventilation is done to increase the PaCO2 and the Valsalva maneuver may be used in Trendelenburg position [15]. High index of suspicion is required to diagnose an anaphylactic reaction and to manage it byearly aggressive surgical treatment and delivering 100% oxygen with epinephrine infusion and massive fluid resuscitation. To prevent and treat the refractory hypotension, prophylactic hydrocortisone supplementation is also recommended [15]. The proper protocol should be followed as represented in the schematic flowchart (Figure 5).
3.4.3. Complications
An intra-operative rupture of hydatid cysts can lead to fatal anaphylactic reaction and a high chance of recurrence [12]. The reported recurrence rate in the brain due to cyst rupture at surgery is reported 40.7% [1]. Mainly reported post-operative complications are hemorrhage, seizures, subdural effusion, porencephalic cyst, hydrocephalus, pneumocephalus, and focal neurological deficits, which sometime may need further intervention [7]. The space left after the excision of large hydatid cysts may lead to fatal complications, such as subdural hematomas, hyperpyrexia, cerebral edema, cortical collapse, or cardiorespiratory failure, in the early post-operative days. In late post-operative days the rate of complication such as subdural effusion and the porencephalic cyst. Cortical collapse associated with mortality is around 0.07 [16]. Majority of cases with neurological deficits improved completely as Hilmani et al. described 90% recovery in the neurological deficits in their case series [5].
4. Conclusion
In endemic countries (even in non-endemic countries due to migration), while considering differentials for cystic masses of the brain, the hydatid cyst disease has an important place. Its rupture can be detrimental for the patient, so proper protocol should be followed for complete excision to prevent anaphylactic reaction and dissemination.
Ethical Considerations
Compliance with ethical guidelines
This research was approved by the Ethics Committee of SMS Hospital, Jaipur, India.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
All authors have contributed equally to the manuscript.
Conflict of interest
The authors declare no conflict of interest.
References
Khalifa RMA, Mahmoud AE, Othman RM. Spotlight on the hydatid cyst and whether its location is accidental or target. Parasitol United Journal. 2015; 8(1):4-13. [DOI:10.4103/1687-7942.163403]
Nemati A, Kamgarpour A, Rashid M, Nazari SS. Giant cerebral hydatid cyst in a child: A case report and review of the literature. British Journal of Medical Practitioners (BJMP). 2010; 3(3):a338.
Luo K, Luo DH, Zhang TR, Wen H. Primary intracranial and spinal hydatidosis: A retrospective study of 21 cases. Pathog Glob Health. 2013; 107(2):47-51. [DOI:10.1179/2047773213Y.0000000072] [PMID] [PMCID]
Tuzun Y, Kadioglu HH, Izci Y, Suma S, Keles M, Aydin IH. The clinical, radiological, and surgical aspects of cerebral hydatid cysts in children. Pediatric Neurosurgery. 2004; 40(4):155-60. [DOI:10.1159/000081932] [PMID]
Hilmani S. Brain hydatid cyst. In: Echinococcosis. Alfonso J. Rodriguez-Morales. IntechOpen; 2015. [DOI:10.5772/60820]
Gupta S, Desai K, Goel A. Intracranial hydatid cyst: A report of five cases and review of the literature. Neurol India. 1999; 47:214
Ersahin Y, Mutluer S, Guzelbag E. Intracranial hydatid cysts in children. Neurosurgery. 1993; 33(2):219-24. [DOI:10.1097/00006123-199308000-00006] [PMID]
Debourgogne A, Goehringer F, Umhang G, Gauchotte G, Hénard S, Boué F, et al. Primary cerebral alveolar echinococcosis: Mycology to the rescue. Journal of Clinical Microbiology. 2014; 52(2):692-94. [DOI:10.1128/JCM.02843-13] [PMID] [PMCID]
Alok R, Mahmoud J. Successful surgical treatment of a brain stem hydatid cyst in a child. Case Reports in Surgery. 2020; 2020:1-3. [DOI:10.1155/2020/5645812] [PMID] [PMCID]
Imperato A, Consales A, Ravegnani M, Castagnola E, Bandettini R, Rossi A. Primaryhydatid cyst of the brain in a child. Polish Journal of Radiology. 2016; 81:578-82. [DOI:10.12659/PJR.898619] [PMID] [PMCID]
Altibi AM, Qarajeh RA, Belsuzarri TA, Maani W, Kanaan TM. Primary cerebral echinococcosis in a child: A case report - Surgical technique, technical pitfalls, and video atlas. Surgical Neurology International. 2016; 7:S893-8. [DOI:10.4103/2152-7806.194512] [PMID] [PMCID]
Senapati SB, Parida DK, Pattajoshi AS, Gouda AK, Patnaik A. Primary hydatid cyst of the brain: Two cases report. Asian Journal of Neurosurgery. 2015; 10(2):175-6. [DOI:10.4103/1793-5482.152109] [PMID] [PMCID]
Lotfinia I. Central nervous system hydatid disease. [Internet]. 2017 [Cited 2017 Feb 23 ]; Available from: https://smjournals.com/ebooks/monographs/chapters/MONO-17-02.pdf
Arora SK, Aggarwal A, Datta V. Giant primary cerebral hydatid cyst: A rare cause of childhood seizure. Journal of Pediatric Neurosciences. 2014; 9(1):73-5. [DOI:10.4103/1817-1745.131495] [PMID] [PMCID]
Nashibi M, Tafrishinejad A, Hussain Khan Z. Deep seated cerebral hydatid cyst and it’s anesthetic considerations: A case report. Archives of Neuroscience. 2020; 7(1):e100044. [DOI:10.5812/ans.100044]
Cavusoglu H, tuncer C ozdilmac A, Aydin Y. Multiple intracranial hydatid cysts in a boy. Turkish Neurosurgery. 2009; 19(2):203-7. [PMID]
Type of Study: Case report |
Subject:
Basic Neurosurgery
Send email to the article author
| Rights and Permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |